JOINTS 2025;
3: e1601
DOI: 10.26355/joints_20259_1601
Arthroscopic management of hip synovial chondromatosis: a systematic review of clinical outcomes and recurrence rates
Topic: Hip
Category: Systematic Review
Abstract
OBJECTIVE: Synovial chondromatosis (SC) of the hip is a rare benign condition caused by intra-articular cartilaginous nodules, which may lead to secondary osteoarthritis (OA). Arthroscopic treatment (AT) is increasingly used as a minimally invasive option. This systematic review aimed to evaluate the efficacy, safety, and recurrence rates of AT for hip SC, focusing on clinical outcomes, complications, and the need for revision surgery.
MATERIALS AND METHODS: A systematic literature search was performed across PubMed, Scopus, Embase, MEDLINE, and Cochrane databases up to December 2024, following PRISMA guidelines. Clinical studies on arthroscopic treatment of hip SC in humans, published from 2000 to 2024, with ≥22 months of follow-up and levels of evidence I-IV were included. Thirteen studies with 369 patients were analyzed. Methodological quality was assessed using the Oxford level of evidence (LoE) and modified Coleman Methodology Score (mCMS). Extracted data included demographics, surgical technique, clinical outcomes, complications, and recurrence.
RESULTS: The review included 369 patients (mean age 26.7-45.1 years; predominantly male). Arthroscopic treatment led to significant improvements in functional outcomes, with marked increases in modified Harris Hip Score (mHHS), International Hip Outcome Tool (iHOT12), Non-Arthritic Hip Score (NAHS) scores, and pain reduction on Visual Analogue Scale (VAS). Patient-reported satisfaction ranged from 75% to 100%. The overall recurrence rate was 22.7%, with 38 patients undergoing repeated arthroscopy and 44 requiring open revision surgery. Progression to end-stage OA occurred in 7.3% of cases, necessitating total hip arthroplasty. Reported complications were infrequent and mostly minor, including transient neuropraxia and perineal numbness. Synovectomy combined with loose body removal provided durable clinical benefit in most patients, particularly when complete debridement was achieved.
CONCLUSIONS: Arthroscopic treatment is a safe and effective option for hip SC, providing durable symptom relief, high satisfaction, and acceptable recurrence. Accurate diagnosis, staging, and patient selection are essential. Standardized protocols are needed to optimize outcomes.
Introduction
Synovial chondromatosis (SC) is a rare, benign condition of unknown etiology, characterized by the formation of cartilaginous nodules within the synovial membrane of joints, bursae, or tendon sheaths1,2. The disease typically progresses through three stages: initial synovial proliferation without loose bodies, a transitional phase with both active synovitis and loose bodies, and a late phase dominated by intra-articular loose bodies with quiescent synovium1. These nodules can detach and migrate within the joint, potentially leading to mechanical damage of the articular cartilage and secondary osteoarthritis (OA)2. SC most commonly affects males between the third and fifth decades of life, with a male-to-female ratio of approximately 2:13.
While the knee is the most frequently involved site, SC can also affect other joints, including the hip, elbow, wrist, and temporomandibular joint1. Although typically intra-articular, extra-articular manifestations involving tendon sheaths and bursae have been reported2. In the hip, SC presents with non-specific symptoms such as groin pain, crepitus, reduced range of motion (ROM), and joint tenderness, often mimicking early OA1,3. Conventional radiographs may reveal calcified nodules in approximately 70% of cases4, though early-stage disease may lack detectable calcifications5. Advanced imaging modalities like computed tomography (CT) or magnetic resonance imaging (MRI) are indicated when standard radiographs are inconclusive5. MRI, in particular, provides superior soft tissue contrast, allowing for the identification of non-calcified loose bodies, synovial thickening, and disease extent6.
Open surgical dislocation of the hip, as described by Ganz et al7, remains a valid approach for SC treatment, offering direct visualization of the joint while preserving the femoral head blood supply. However, the advent of advanced arthroscopic techniques (ATs) has led to a paradigm shift, favoring minimally invasive management due to lower morbidity and faster recovery8. Arthroscopic procedures typically involve the removal of intra-articular loose bodies, with partial or complete synovectomy depending on the extent of synovial involvement9,10. Loose body removal alone may suffice in limited disease, whereas extensive synovial proliferation requires synovectomy to reduce recurrence risk and achieve durable symptom relief11. Arthroscopic treatment has demonstrated promising outcomes in terms of pain reduction, functional improvement, and recurrence prevention9-11.
The aim of this systematic review is to critically evaluate the clinical outcomes, complication rates, and risk of recurrence associated with arthroscopic treatment of hip SC, with the goal of defining its effectiveness and indications based on current evidence.
Materials and Methods
Research Question
This systematic review was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines to ensure the rigorous identification and selection of relevant studies12. Two independent reviewers (RGV and AE) performed the search and screening processes to minimize potential bias. In case of disagreement, a third reviewer (FG) was consulted to resolve any uncertainties.
Inclusion and Exclusion Criteria
Studies were eligible for inclusion if they involved patients undergoing arthroscopic surgery for hip SC. To be considered, studies had to involve human subjects, be published between 2000 and December 2024, and report a minimum follow-up of 22 months, with a level of evidence (LoE) ranging from 1 to 4. Excluded papers comprised biochemical studies, in vitro research, case reports, editorials, book chapters, technical notes, preclinical studies, and studies with LoE 5.
Search Strategy and Study Screening
A comprehensive search was conducted in five databases (PubMed, Scopus, Embase, Cochrane, and MEDLINE) using the following MeSH terms: ((synovial chondromatosis) OR (chondromatosis)) AND (arthroscopic*) AND (hip). A total of 364 articles were identified. After removing duplicates, 184 articles remained. Titles and abstracts were screened, resulting in the exclusion of 168 studies. Sixteen articles underwent full-text review, of which 13 met the inclusion criteria and were selected for qualitative analysis. The selected studies provided data on patient positioning, arthroscopic portals, postoperative protocols, functional outcomes, time to symptom resolution, complications, and revision rates in patients treated with ATs for hip SC. The selection process is illustrated in the PRISMA flowchart (Figure 1).
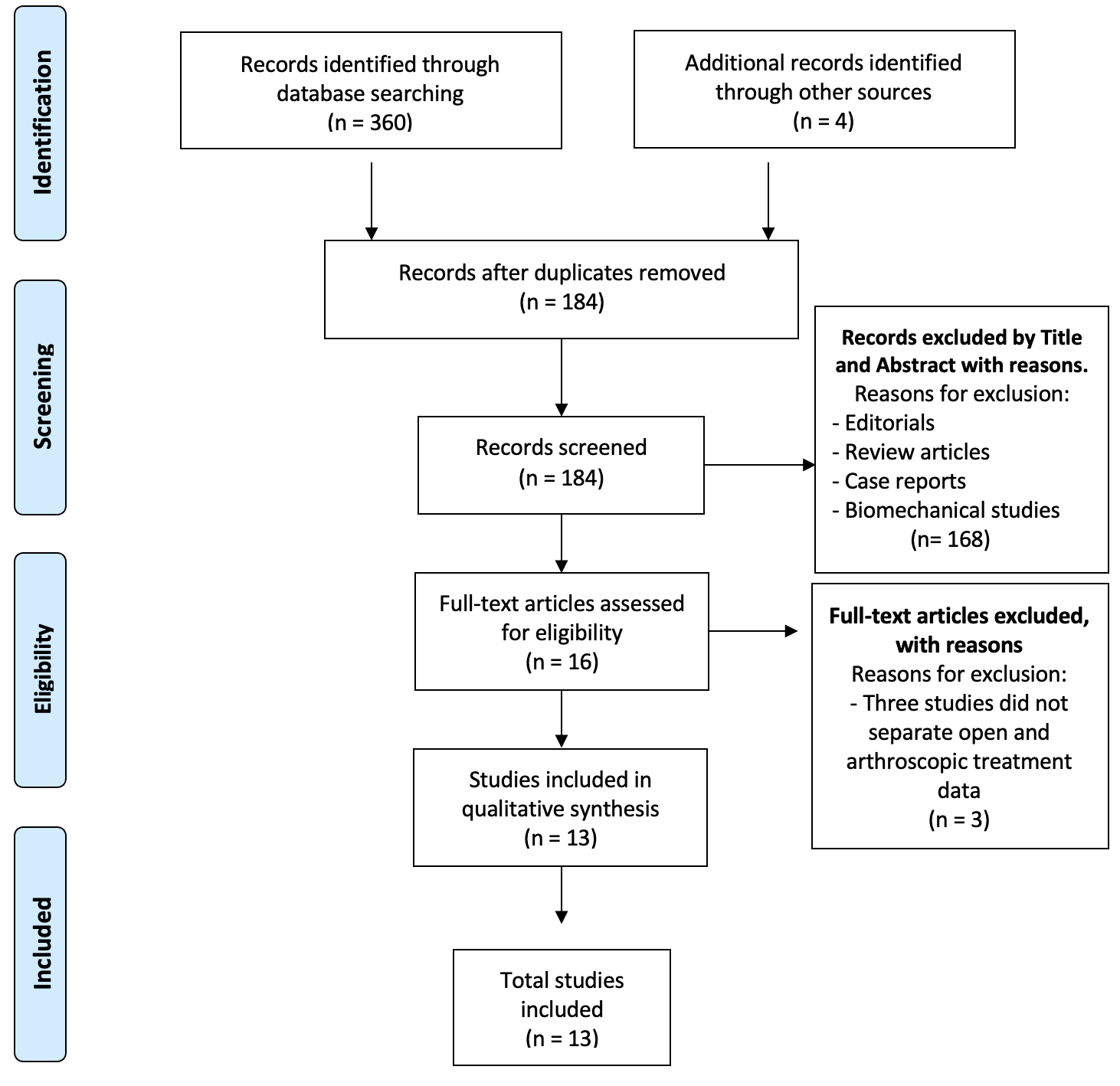
n: number.
Methodological Quality Assessment
The quality of the included studies was evaluated using the 2011 Oxford Centre for Evidence-Based Medicine Levels of Evidence framework13. Studies were graded from level 1 (highest) to level 5. Retrospective studies were further assessed using the modified Coleman Methodology Score (mCMS), as adapted from Ramponi et al14 (Figure 2). Complications were categorized according to the Clavien-Dindo classification15. This systematic review was registered in the International Registry of Systematic Reviews (PROSPERO), under the ID CRD420250652745, in February 202516.
Figure 2. Retrospective studies analysis performed through the modified Coleman Methodology Score.
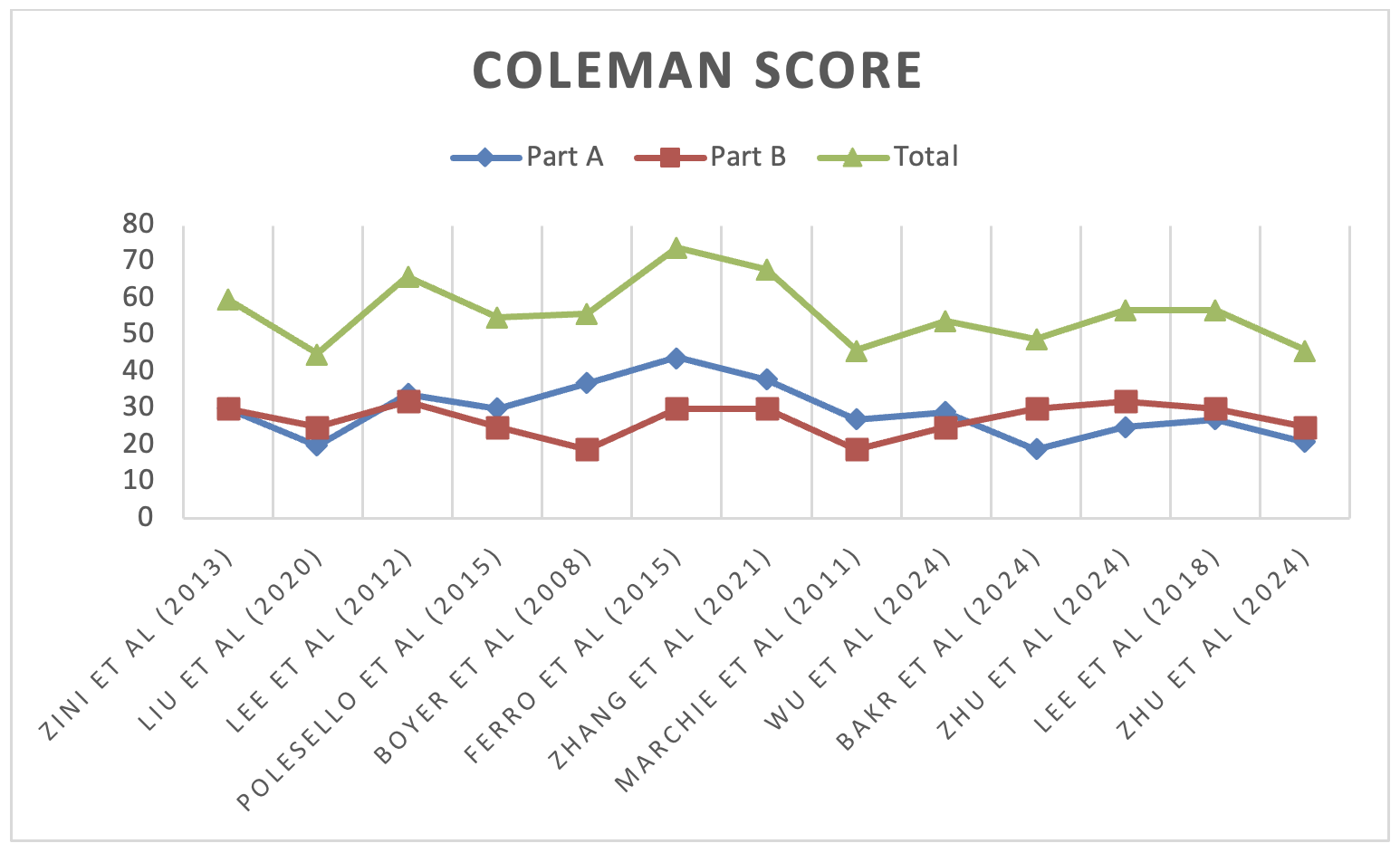
Data Extraction
Data from the included studies were extracted systematically using a standardized template. Extracted variables included authorship, year of publication, study design, sample size, mean patient age, radiographic findings, arthroscopic portals used, and mean operative time. Clinical outcomes were assessed using pre- and postoperative scores, including the modified Harris Hip Score (mHHS), Harris Hip Score (HHS), Non-Arthritic Hip Score (NAHS), Visual Analogue Scale (VAS), Western Ontario and McMaster Universities Arthritis Index (WOMAC), Short Form-12 (SF12), International Hip Outcome Tool (iHOT12), Hip Disability and Osteoarthritis Outcome Score (HOOS), Hip Sports Activity Scale (HSAS), Hip Outcome Score Sport-Specific Subscale (HOS-SSS), Hip Outcome Score for Activities of Daily Living (HOOS-ADL), Japanese Orthopedic Association (JOA) score, EuroQoL-5 Dimension Questionnaire (EQ-5D), Hip-Related Quality of Life (QoL) score, and University of California Los Angeles (UCLA) activity score. Postoperative protocols, complications, and revision rates were also recorded. The structured template facilitated the organized and comprehensive analysis of the collected data.
Data Analysis
Data analyses were conducted using R software (2022 version 4.1.3, R Core Team, Vienna, Austria). Given the expected clinical and methodological heterogeneity, we prespecified a narrative synthesis and did not perform a meta-analysis. Continuous outcomes were extracted as means and standard deviations (SDs) for each study and are reported individually. There was no pooling of data across studies, imputation of variances, or transformation of medians/ranges. For event outcomes (such as recurrence, complications, and conversion to total hip arthroplasty), we present descriptive pooled proportions, calculated as the sum of events divided by the total number of hips among the studies reporting that endpoint. The 95% confidence intervals (CIs) were determined using the Wilson method; therefore, the denominators vary by endpoint.
Results
Thirteen studies9-11,17-26 (LoE 4), published between 2008 and 2024, met all inclusion criteria and were included in the qualitative analysis. All were retrospective, except for those by Ferro et al22 and Polesello et al25, which were prospective. A total of 369 patients were analyzed. Among the 12 studies reporting sex distribution, 198 were males and 150 females, with a mean patient age ranging from 26.7 to 45.1 years. Eight studies10,17,18,20,21,23-25 reported the side affected: 99 patients had left-sided involvement, and 139 had right-sided involvement. In eight studies9-11,17,18,21,23,24, the mean time from symptom onset to surgery ranged from 2.5 to 52 months. Body mass index (BMI) or weight was reported in four studies9,10,18,19, with values ranging from 23 to 24.6 kg/m2.
Diagnosis
The diagnosis of hip SC was established based on medical history, physical examination, and imaging – namely anteroposterior and lateral radiographs, CT scans, arthrograms, or MRI. Eleven studies9,11,17-21,23-26 reported clinical symptoms such as hip pain, mechanical symptoms (limping, crepitus), and restricted ROM. Seven studies9,11,17,18,21,23,24 described the radiologic diagnostic modalities. Cartilage damage of the femoral head and acetabulum was classified using the Tönnis grading system in six studies9,17-19,22,24, while Milgram’s histological staging was reported in seven9,18,21,23-26. Six studies9,17-19,22,24 also noted concomitant joint conditions. An overview of diagnostic features is provided in Table 1.
Surgical Technique
All patients underwent hip arthroscopy, with or without traction, for primary SC. Synovectomy and loose body removal techniques were described in sufficient detail to achieve the maximum Coleman score (Figure 2). Patients were positioned supine in all studies except Marchie et al11, who used the lateral decubitus position. Twelve studies9-11,17-24,26 specified the arthroscopic portals used (anterolateral, mid-anterior, or posterolateral), and 119-11,17-24 detailed the arthroscopic techniques. Four studies11,17,19,24 reported surgery durations ranging from 80 to 144 minutes (Table 2).
Postoperative Rehabilitation
Postoperative rehabilitation protocols are summarized in Table 2. Eight studies9,11,17,18,20,22,24,26 described rehabilitation programs and weight-bearing restrictions in detail. Follow-up periods across the 13 studies ranged from 17.1 to 104.9 months.
Final Reported Outcomes
Eleven studies9,10,17-22,24-26 reported subjective patient outcomes using scores such as mHHS, VAS, NAHS, iHOT12, HSAS, HOS-SSS, HOOS-ADL, JOA, EQ-5D, SF-12, Hip-Related QoL, and UCLA activity scores. A positive outcome was defined as full symptom resolution without residual synovitis or mobile loose bodies at final follow-up. Patient satisfaction ranged from 75% to 100% (Table 3).
Complications
Recurrence was summarized as a descriptive pooled proportion (events/hips) across studies that reported the endpoint, which was 22.8% (84/369; 95% CI, 18.8-27.3%). Conversion to total hip arthroplasty (THA) occurred in 7.3% (27/369; 95% CI 5.1-10.4%). These values are descriptive aggregates, not random-effects pooled estimates, and should be interpreted with consideration of between-study heterogeneity; per-study data are reported in Table 3. Major complications (Clavien-Dindo IIIb) included inadequate loose-body removal, which required revision (repeat arthroscopy, n=38; open revision, n=44). Three patients experienced transient neurological symptoms (perineal numbness, pedal paresthesia, or femoral nerve neuropraxia).
Discussion
The most relevant finding of this systematic review is that arthroscopic treatment (AT) of hip SC achieves high patient satisfaction with low recurrence and complication rates.
As previously reported in the literature, SC predominantly affects males, with a male-to-female ratio of 1.3:1 – slightly lower than the 2:1 ratio typically reported for SC in all joints3. Patient age ranged from 13 to 81 years, with a prevalence in the third and fourth decades. These findings underscore the importance of early diagnosis and appropriate treatment to minimize recurrence and delay progression to OA. Nevertheless, moderate to severe OA can negatively impact long-term outcomes of AT and must be carefully evaluated when planning treatment27.
The most frequently reported symptoms at onset were groin pain and limited ROM, common to many hip pathologies, and thus potentially delaying diagnosis. The long symptom duration before surgery, ranging from 3 to 180 months, highlights this diagnostic challenge. Imaging plays a key role in differential diagnosis; since intra-articular loose bodies may not be visible on early radiographs, advanced imaging – preferably MRI – is essential for accurate diagnosis and surgical planning5.
Surgical treatment in early-stage SC generally provides satisfactory outcomes; however, proper patient selection and thorough assessment of joint status remain essential. Removal of loose bodies may offer symptomatic relief, but in cases of coexisting OA, hip preservation surgery may fail. THA remains the best option for advanced joint degeneration, ensuring long-term symptom resolution28.
The debate between open surgery and AT continues. Surgical hip dislocation (SHD), as described by Ganz7, enables full access to the joint while preserving femoral head vascularity, thus reducing the risk of avascular necrosis. This approach allows comprehensive removal of loose bodies, evaluation of joint damage, and treatment of associated conditions such as labral tears or cam deformities. However, SHD is more invasive, carries a higher risk of soft tissue trauma, and may complicate future THA due to scar tissue formation.
Recent technical advancements and the availability of dedicated instruments have established hip arthroscopy as a valid alternative for SC management29. While both approaches require specific expertise and present steep learning curves, AT offers the advantages of minimal invasiveness and faster recovery. Criticisms of AT include the potential for recurrence due to incomplete loose body removal, often limited by reduced joint visibility, and the theoretical risk of malignant lesion dissemination. Nevertheless, modern instrumentation and multiple arthroscopic portals now permit near-complete visualization of the joint, allowing meticulous removal of loose bodies and minimizing iatrogenic cartilage damage. Additionally, the risk of malignant transformation in SC is extremely low, and the likelihood of tumor spread after arthroscopic capsulotomy is negligible30.
There is currently no universally accepted surgical technique. The approach must be tailored to the location and extent of the loose bodies and to patient positioning. While the supine position is more commonly used, the lateral position may offer the advantage of gravitational pooling of loose bodies toward the fovea, simplifying their identification and removal.
Most included studies had small sample sizes, reflecting the rarity of this disease. Boyer and Dorfmann23 reported the largest cohort treated with AT for hip SC; however, this 2008 study includes patients operated on between 1985 and 2000. Limitations related to outdated imaging, lack of surgical standardization, and variable diagnostic accuracy may have contributed to the relatively poor outcomes observed in that cohort, including high recurrence and complication rates. With modern advancements, clinical results have improved, but there remains a need for protocols tailored to the disease stage.
In addition, case reports and technical notes, such as those by Rath et al31 and Carulli et al32, have described arthroscopic management of hip SC, further underscoring both the technical feasibility and the rarity of this condition. Although informative, these reports were not included in our systematic review due to their study design and limited follow-up, as per our predefined inclusion criteria.
Limitations
This review has several limitations. First, most of the included studies were retrospective, often with small sample sizes and heterogeneous populations in terms of age, symptom duration, disease severity, and concomitant pathologies. Given these sources of heterogeneity, we deliberately refrained from meta-analytic pooling of continuous outcomes and reported study-level results instead. Event outcomes (recurrence, complications, THA) were summarized as descriptive pooled proportions with 95% CIs, which provide an overall orientation but may over- or under-represent individual cohorts. This approach minimizes the risk of misleading precision while preserving transparency of the evidence base. Second, diagnostic strategies varied widely, with some patients being assessed only with radiographs and others undergoing CT or MRI scans. Third, surgical interventions were not standardized, with different combinations of loose body removal and synovectomy. Postoperative rehabilitation protocols also varied significantly according to surgeon preference and intraoperative findings, which may have influenced recovery. Finally, the follow-up duration varied substantially (12-196 months), introducing potential bias and limiting the reliability of long-term outcome comparisons. A uniform clinical and radiological follow-up strategy would greatly enhance the comparability and validity of future data.
Further high-quality research is needed to evaluate the long-term efficacy, safety, and cost-effectiveness of arthroscopic management of hip SC. Large, well-designed randomized controlled trials with homogeneous control groups are essential to clarify the advantages of AT compared to open surgery. Moreover, improved patient stratification based on age, joint status, and disease stage is crucial for selecting the most appropriate treatment. Standardized diagnostic algorithms and postoperative rehabilitation protocols are also required to reduce diagnostic delays and optimize functional recovery.
Conclusions
This systematic review demonstrates that ATs represent a viable and effective treatment option for hip SC, particularly when performed by experienced hip arthroscopists. ATs offer high patient satisfaction, significant functional improvement, and acceptable recurrence rates, while maintaining the advantages of a minimally invasive approach. However, the considerable variability in diagnostic methods, surgical strategies, and postoperative protocols highlights the urgent need for standardized treatment guidelines. In cases of advanced joint degeneration, THA may remain the most appropriate therapeutic alternative.
Conflict of Interest
The authors declare that they have no conflict of interest.
Funding
The authors received no funding for this research
AI Disclosure
The authors declare that artificial intelligence was not utilized to assist in any aspects of this manuscript’s formulation.
Availability of Data and Materials
All data generated or analyzed during this study are included in this manuscript.
Ethics Approval and Informed Consent
Not applicable.
Authors’ Contributions
Riccardo Giai Via: substantial conception/design of work, performed measurements, data collection, statistical analysis, interpretation of data, drafting the work, critically revising the work, manuscript preparation, approving final version for publication, and agreement for accountability of all aspects of work.
Ahmed Elzeiny, Salvatore Pantè, Cristiano De Franco: substantial conception/design of work, interpretation of data for work, revising of the work for important intellectual content, final approval of the version for publication, and agreement to the accountability of all aspects of the work.
Kristijan Zoccola, Alessandro Massè: substantial conception/design of work, revising of the work for important intellectual content, final approval of the version for publication, and agreement to the accountability of all aspects of the work.
Fortunato Giustra, Francesco Bosco, Alessandro Aprato: revising of the work for important intellectual content, manuscript preparation, final approval of the version for publication, and agreement to accountability of all aspects of the work.
ORCID ID
Riccardo Giai Via: 0000-0003-1170-230X
Ahmed Elzeiny: 0009-0000-9528-6723
Salvatore Pantè: 0000-0001-8203-2417
Cristiano De Franco: 0000-0003-1582-7345
Fortunato Giustra: 0000-0001-6386-2933
Francesco Bosco: 0000-0001-8306-1869
Kristijan Zoccola: 0000-0003-4195-2879
Alessandro Massè: 0000-0003-3999-4121
Alessandro Aprato: 0000-0002-2514-4719
References
- Neumann JA, Garrigues GE, Brigman BE, Eward WC. Synovial Chondromatosis. JBJS Rev 2016; 4: e2.
- van der Valk MR, Veltman ES, Assink J, Veen MR. Synovial chondromatosis of the hip, a case report and literature review. J Orthop 2019; 16: 249‑253.
- Adelani MA, Wupperman RM, Holt GE. Benign synovial disorders. J Am Acad Orthop Surg 2008; 16: 268-275.
- McKenzie G, Raby N, Ritchie D. A pictorial review of primary synovial osteochondromatosis. Eur Radiol 2008; 18: 2662-2669.
- Duif C, von Schulze Pellengahr C, Ali A. Primary synovial chondromatosis of the hip – is arthroscopy sufficient? A review of the literature and a case report. Technol Health Care 2014; 22: 667-675.
- Schagemann JC, Hunold P, Russlies M, Mittelstaedt H. Synovial chondromatosis of the hip with atypical MRI morphology and mistakable clinical symptoms – a case report. Acta Orthop 2011; 82: 246-249.
- Ganz R, Gill TJ, Gautier E, Ganz K, Krügel N, Berlemann U. Surgical dislocation of the adult hip a technique with full access to the femoral head and acetabulum without the risk of avascular necrosis. J Bone Joint Surg Br 2001; 83: 1119-1124.
- Giai Via R, Giachino M, Elzeiny A, Aprato A. Arthroscopic Management of Pigmented Villonodular Synovitis of the Hip: A Systematic Review. J Clin Med 2024; 13: 6446.
- Zhu Y, Gao G, Luan S, Xu Y. Longitudinal Assessment of Clinical Outcomes After Arthroscopic Treatment for Hip Synovial Chondromatosis and the Effect of Residual Loose Bodies: Minimum 4-Year and 8-Year Follow-up. Am J Sports Med 2024; 52: 2306-2313.
- Zhang X, Gao G, Wang J, Xu Y. Clinical Outcomes after Arthroscopic Treatment of Synovial Chondromatosis in the Hip. Cartilage 2021; 13: 1324S-1330S.
- Marchie A, Panuncialman I, McCarthy JC. Efficacy of hip arthroscopy in the management of synovial chondromatosis. Am J Sports Med 2011; 39 Suppl: 126S-131S.
- Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021; 372: n71.
- Burns PB, Rohrich RJ, Chung KC. The levels of evidence and their role in evidence-based medicine. Plast Reconstr Surg 2011; 128: 305-310.
- Ramponi L, Yasui Y, Murawski CD, Ferkel RD, DiGiovanni CW, Kerkhoffs GMMJ, Calder JDF, Takao M, Vannini F, Choi WJ, Lee JW, Stone J, Kennedy JG. Lesion size is a predictor of clinical outcomes after bone marrow stimulation for osteochondral lesions of the talus: A systematic review. Am J Sports Med 2017; 45: 1698-1705.
- Dindo D, Demartines N, Clavien PA. Classification of surgical complications: A new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 2004; 240: 205-213.
- Sideri S, Papageorgiou SN, Eliades T. Registration in the international prospective register of systematic reviews (PROSPERO) of systematic review protocols was associated with increased review quality. J Clin Epidemiol 2018; 100: 103-110.
- Zini R, Longo UG, de Benedetto M, Maffulli N, Denaro V. Arthroscopic management of primary synovial chondromatosis of the hip. Arthroscopy 2013; 29: 420-426.
- Zhu Y, Zhang X, Wang J, Gao G, Xu Y. Revision hip arthroscopy for hip synovial chondromatosis is effective despite inferior postoperative clinical outcomes compared to patients undergoing primary hip arthroscopy: A matched control study with minimum 2-year follow-up. J Orthop Surg 2024; 19: 819.
- Lee YK, Moon KH, Kim JW, Hwang JS, Ha YC, Koo KH. Remaining loose bodies after arthroscopic surgery including extensive capsulectomy for synovial chondromatosis of the hip. Clin Orthop Surg 2018; 10: 393-397.
- Wu W, Liu M, Zhou C, Chen D, Zhang Q, He H, Zhang J. Efficacy of outside-in hip arthroscopy without traction in the treatment of hip synovial osteochondromatosis. Orthop Surg 2024; 16: 2862-2867.
- Bakr HMA, Abdelkader SM, Metwally O. Is arthroscopic management of synovial chondromatosis of the hip enough?J Arthrosc Jt Surg 2024; 11: 144-148.
- Ferro FP, Philippon MJ. Arthroscopy provides symptom relief and good functional outcomes in patients with hip synovial chondromatosis. J Hip Preserv Surg 2015; 2: 265-271.
- Boyer T, Dorfmann H. Arthroscopy in primary synovial chondromatosis of the hip: Description and outcome of treatment. J Bone Joint Surg Br 2008; 90: 314-318.
- Lee JB, Kang C, Lee CH, Kim PS, Hwang DS. Arthroscopic treatment of synovial chondromatosis of the hip. Am J Sports Med 2012; 40: 1412-1418.
- Polesello GC, Ono NK, Honda EK, Guimaraes RP, Ricioli W Jr, Queiroz MC, Guimaraes SM. Arthroscopic treatment of synovial osteochondromatosis of the hip. Rev Bras Ortop 2015; 44: 320-323.
- Liu Y, Li J, Ma N, He R, Zhao L. Arthroscopic treatment of synovial chondromatosis of hip joint. J Orthop Surg Res 2020; 15: 405.
- Domb BG, Gui C, Lodhia P. How much arthritis is too much for hip arthroscopy: A systematic review. Arthroscopy 2015; 31: 520-529.
- Learmonth ID, Young C, Rorabeck C. The operation of the century: Total hip replacement. Lancet 2007; 370: 1508-1519.
- Colvin AC, Harrast J, Harner C. Trends in hip arthroscopy. J Bone Joint Surg Am 2012; 94: e23.
- Krych AJ, Odland AN, Rose PS, Kasperbauer JL, Wenger DE, Van Wymelbeke DM, Levy BA. Oncologic conditions that simulate common sports injuries. J Am Acad Orthop Surg 2014; 22: 223-234.
- Rath E, Amar E, Doron R, Matsuda DK. Hip arthroscopy for synovial chondromatosis: Tips and tricks. Arthrosc Tech 2014; 3: e709-e712.
- Carulli C, Schiavo A, Rigon A, De Marchi W, Innocenti M, Meccariello L, Innocenti M. Rare and uncommon diseases of the hip: Arthroscopic treatment. Med Glas (Zenica) 2021; 18: 293-298.
To cite this article
Arthroscopic management of hip synovial chondromatosis: a systematic review of clinical outcomes and recurrence rates
JOINTS 2025;
3: e1601
DOI: 10.26355/joints_20259_1601
Publication History
Submission date: 27 Jun 2025
Revised on: 31 Jul 2025
Accepted on: 29 Aug 2025
Published online: 15 Sep 2025