JOINTS 2025;
3: e1651
DOI: 10.26355/joints_20259_1651
Minimally invasive treatment of calcaneus fracture
Topic: Ankle
Category: Original article
Abstract
OBJECTIVE: The management of calcaneal fractures remains a topic of ongoing debate in the literature. This study aims to compare the functional outcomes of patients treated with an external fixator (EF) after percutaneous reduction with those treated using minimally invasive open reduction and internal fixation with a locking plate (LP).
PATIENTS AND METHODS: This retrospective study included 27 patients with 28 calcaneal fractures (Sanders type II and III), 12 with EF and 16 with LP, treated at Carlo Poma Hospital (Mantua, Italy) from 2014 to 2018. The average patient age at the time of surgery was 46.3 years. The mean follow-up period was 123.3 months for the EF group and 101.2 months for the LP group. American Orthopaedic Foot and Ankle Society (AOFAS) scores were recorded, patients’ satisfaction based on AOFAS scores was considered, and all underwent CT scans to assess calcaneal geometry, subtalar joint restoration, and post-traumatic arthritis.
RESULTS: The mean AOFAS score for patients treated with EF was 74.1 (range 37-100). Of these, 66.7% rated their results as excellent or good. The mean AOFAS score for patients treated with LP was 76 (range 55-88), with 75% reporting excellent or good outcomes. The mean increase in Böhler’s angle was 18.9° following EF and 15.9° following LP. One case of algodystrophy and one case of secondary subtalar arthrodesis were observed.
CONCLUSIONS: The functional and radiographic outcomes of the two surgical methods are comparable. Both LP and EF offer the benefits of minimally invasive procedures, enabling adequate fracture reduction and restoration of calcaneal volume. Minimally invasive reduction and osteosynthesis yield results similar to open surgery while reducing postoperative complications.
Introduction
The calcaneus is the most commonly fractured bone in the foot, with 65-70% of fractures being intra-articular1. The management of calcaneal fractures has been controversial for over a century2-8. Despite advancements in diagnostic and therapeutic techniques, complications persist following open reduction and internal fixation9,10.
Minimally invasive techniques aim to restore joint function and promote healing with fewer complications, offering an alternative treatment for displaced intra-articular calcaneal fractures11.
Displaced calcaneal fractures typically occur in young and middle-aged male industrial workers12. Approximately 20% of patients with lower extremity fractures are unable to return to work one year after the injury, and few patients resume their previous level of activity or sport following an intra-articular calcaneal fracture12,13.
Patients who sustain displaced intra-articular calcaneal fractures exhibit poorer general health status (as assessed by the SF-36 questionnaire) compared to those who have suffered myocardial infarctions or undergone organ transplants14.
In literature, several surgical techniques are described, from the extensile lateral approach to the minimally invasive. Our clinical-surgical experience has always been based on minimally invasive surgery, according to the advantages that this entails. Over the years, at our hospital, we have employed two different techniques (external and percutaneous fixation) based on the experience of the operating surgeons (MB and AP).
This study aims to evaluate the long-term outcomes of two different surgical treatments for Sanders type II and III calcaneal fractures using percutaneous and minimally invasive techniques: locking plates (LP) with a sinus tarsi approach and external fixation (EF).
Patients and Methods
This retrospective study included 27 patients with 28 Sanders type II or III calcaneal fractures, treated at Carlo Poma Hospital (Mantua, Italy) from January 2014 to December 2018.
The study protocol was approved by the local Ethics Committee (Val Padana 39/2018) on June 19, 2019.
The data were collected from a minimum 6-year follow-up (range 6-10 years).
The patients’ ages ranged from 21 to 72 years (mean 46.3) at the time of surgery, with 16 males and 11 females. Fifteen fractures occurred in the right heel, and 13 in the left (Table 1). The fractures resulted from falls in 15 cases and motor vehicle accidents in 12.
The first 12 fractures were treated with percutaneous reduction and EF (Orthofix® mini-fixator, Figure 1), while the subsequent 16 fractures were treated with percutaneous plate fixation (Zimmer-Biomet®, Figure 2) using a minimally invasive sinus tarsi approach. Preoperative CT scans were performed for surgical planning.
Fractures were classified as type II (6 cases) and type III (22 cases) according to the Sanders classification15. Inclusion criteria were calcaneus height loss >1.5 cm, subtalar joint displacement >1 mm, and varus malalignment >5°. Exclusion criteria included Sanders type I and IV fractures, compound fractures, follow-up <6 years, associated long-bone fractures, and patients under 16 or over 75 years of age.
The mean follow-up period was 123.3 months for the EF group and 101.2 months for the LP group.
Böhler’s and Gissane’s angles16,17 were measured on the pre- and post-operative lateral radiographs (Figure 3a-d).
Figure 1. Orthofix® mini-fixator.

Figure 2. Zimmer-Biomet® mini-invasive plate.
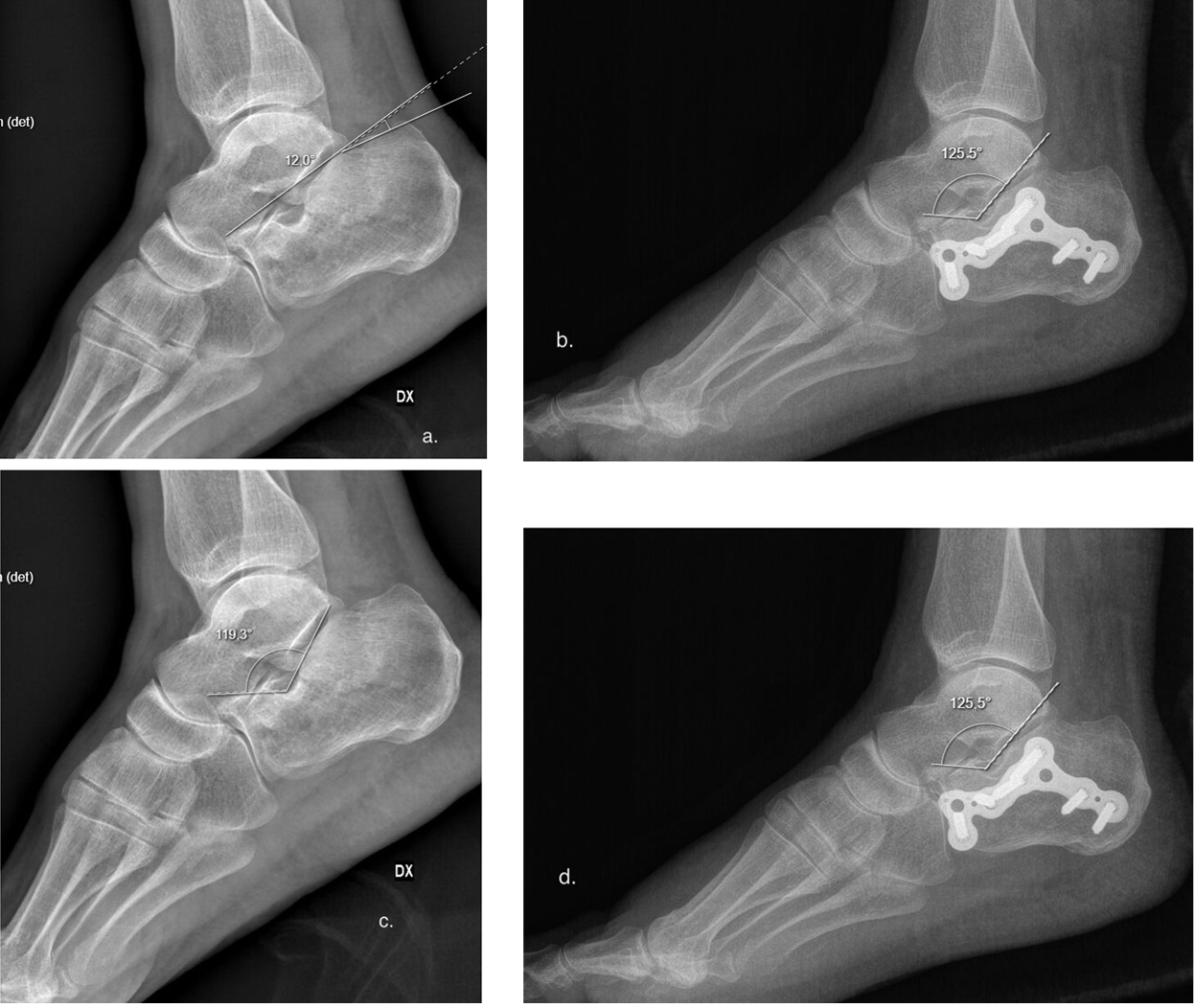
Figure 3. a, preoperative and (b) postoperative X-ray with Böhler’s angle measurement. c, preoperative and (d) postoperative X-ray with Gissane’s angle measurement.
Surgical Techniques
Patients were positioned in the lateral decubitus position to expose the lateral surface of the heel. The procedure was performed under general or locoregional anesthesia with an Esmarch tourniquet.
In the sinus tarsi approach, a 4 cm incision is started just below the tip of the lateral malleolus, in line with the anterior malleolar cortex, heading towards the base of the fourth metatarsal. The next step is to bluntly dissect soft tissues above the peroneal tendons, avoiding injury to either the tendons or the sural nerve. The lateral wall of the calcaneus is then bluntly dissected using a large Cobb elevator, allowing for plate insertion and the restoration of the subtalar articular surface and calcaneal volume. Provisional fixation was achieved with K-wires, and the plate was inserted using a targeting guide. Percutaneous screws were then placed under guidance (Figure 4a-b).
For external fixation, a 1 cm lateral incision was made over the sinus tarsi, and a small lever was used for percutaneous reduction. Two pins were placed in the main fracture fragments, and the mini fixator body was used to position additional pins based on the fracture pattern. After applying the fixator, further reduction and elevation of the fracture fragment were performed.
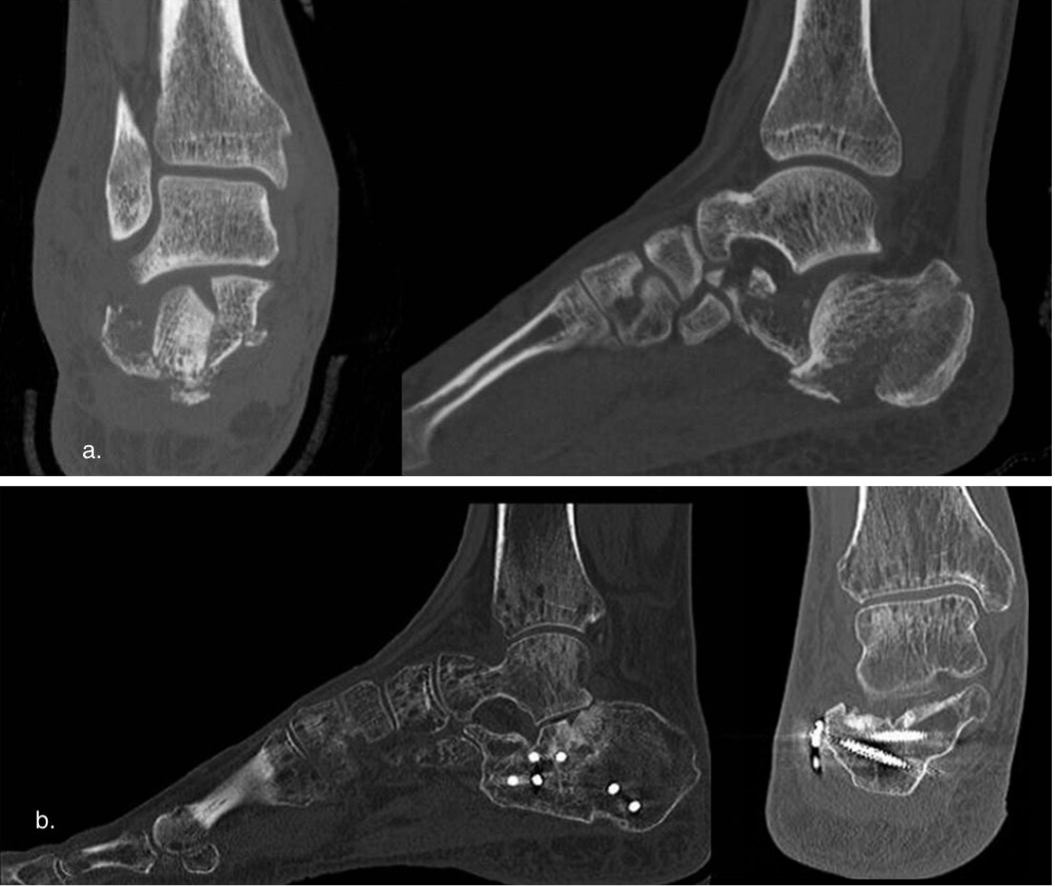
Figure 4. LP clinical case. a, preoperative CT scan, man 46 y. b, CT scan at last follow-up (72 months).
All surgeries were performed by experienced surgeons. The operations were completed within 11 days post-trauma (mean 92.3 minutes for LP, range 60-130 minutes; 76.7 minutes for EF, range 45-115 minutes). The average hospital stay was 8.5 days (range 4-15) for the EF group and 7.2 days (range 3-14) for the LP group (Table 1).
Postoperatively, patients treated with LP were immobilized in a short-leg cast for 4 weeks, followed by partial weight-bearing for another 3 weeks. EF-treated patients began passive and active ankle mobilization on day 1. The external fixator was kept for an average of 7 weeks (range 6-8), with full weight-bearing resuming after 8-12 weeks.
The final follow-up included clinical and radiographic examinations (anteroposterior and lateral ankle radiographs, axial calcaneus views) at 6 weeks, 12 weeks, 6 months, and 12 months, as well as the final follow-up. American Orthopaedic Foot and Ankle Society (AOFAS) scores were recorded at each follow-up. CT scans were performed in all patients at the follow-up.
Statistical Analysis
Statistical analysis using Student’s t-test was performed, and a value of p≤0.05 was considered statistically significant.
| External fixation | MIS | |
| Sex | 5 females, 7 males | 6 females, 9 males |
| Side | 5 R, 7 L | 10 R, 6 L (1 both sides) |
| Sanders II | 3 | 3 |
| Sanders III | 9 | 13 |
| Mean age (range) | 45.2 years (21-63) | 47 years (22-72) |
| Hospital stay (range) | 8.5 days (4-15) | 7.2 days (3-14) |
| Operation time (range) | 76.7 minutes (45-115) | 92.3 minutes (60-130) |
Minimally invasive surgery (MIS).
Results
In the EF group, the mean AOFAS score at final follow-up was 74.1 (range 37-100). The data showed good or excellent outcomes in 50% (6 patients), while two (16.7%) expressed fair results, according to AOFAS scores. Six patients (50%) reported good satisfaction, while two (16.7%) expressed fair results. In the LP group, the mean AOFAS score was 76 (range 55-88), with 75% reporting excellent or good results (Table 2). No significant differences in the AOFAS ankle hindfoot scale scores were observed between the two groups (p=0.65).
The median preoperative Böhler’s angle was 14.2° (range 1°-32°) in the EF group, and 14.9° (range 9°-26°) in the LP group. Postoperative Böhler’s angles were 32.6° (range 20°-58°) and 30.8° (range 20°-49°) in the EF and LP groups, respectively, with median increases of 18.9° and 15.9° (Figure 5, Table 3). In both groups, improvement of postoperative Böhler’s angle was statistically significant (p<0.01)
The median preoperative Gissane’s angle was 130.2° (range 107°-180°) in the EF group, and 129.2° (range 104°-180°) in the LP group. Postoperative Gissane’s angles were 115.8° (range 82°-138°) and 116.9° (range 90°-130°) in the EF and LP groups, respectively (Table 3). In both groups, improvement of postoperative Böhler’s angle was statistically significant (p<0.01).
Postoperative complications included one case of algodystrophy in the LP group, resolved with clodronic acid and pulsed magnetic field therapy. Three cases of chronic peroneal tendinitis were resolved by removing the plate and screws after bone healing, and one patient underwent secondary subtalar arthrodesis due to osteoarthritis 3 years after the injury (Figure 6a-c). Only four patients resumed sports activity (two from each treatment group).
Table 2. Patients’ satisfaction at the follow-up time according to AOFAS scores.
| External fixation | MIS | |
| Excellent | 2 (16.7%) | 4 (25%) |
| Good | 6 (50%) | 8 (50%) |
| Fair | 2 (16.7%) | 4 (25%) |
| Poor | 2 (16.7%) |
American Orthopaedic Foot and Ankle Society (AOFAS), minimally invasive surgery (MIS).
Table 3. Preoperative and postoperative angles.
| External fixation | MIS | |||
| Preoperative | Postoperative | Preoperative | Postoperative | |
| Median Bohler’s angle (range) | 14.2°
(1°to 32°) |
32.6°
(20° to 58°) |
14.9°
(9° to 26°) |
30.75°
(20° to 49°) |
| Median Gissane’s angle (range) | 130.2°
(107° to 180°) |
115.8°
(82° to 138°) |
129.2°
(104° to 180°) |
116.9°
(90° to 130°) |
Minimally invasive surgery (MIS).
Figure 5. Increasing in Böhler’s angle.
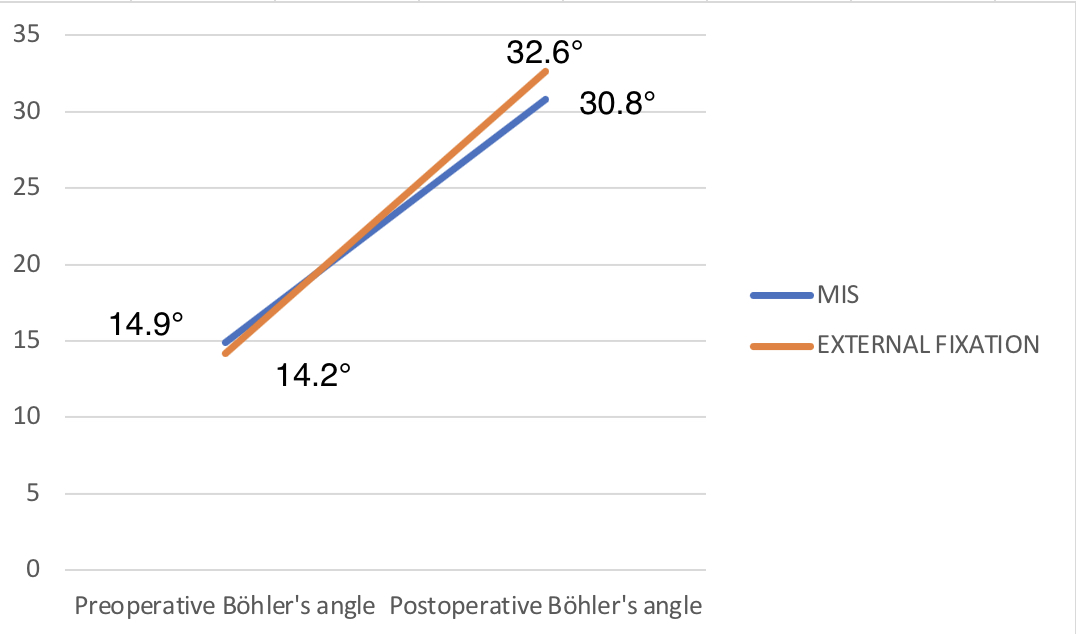
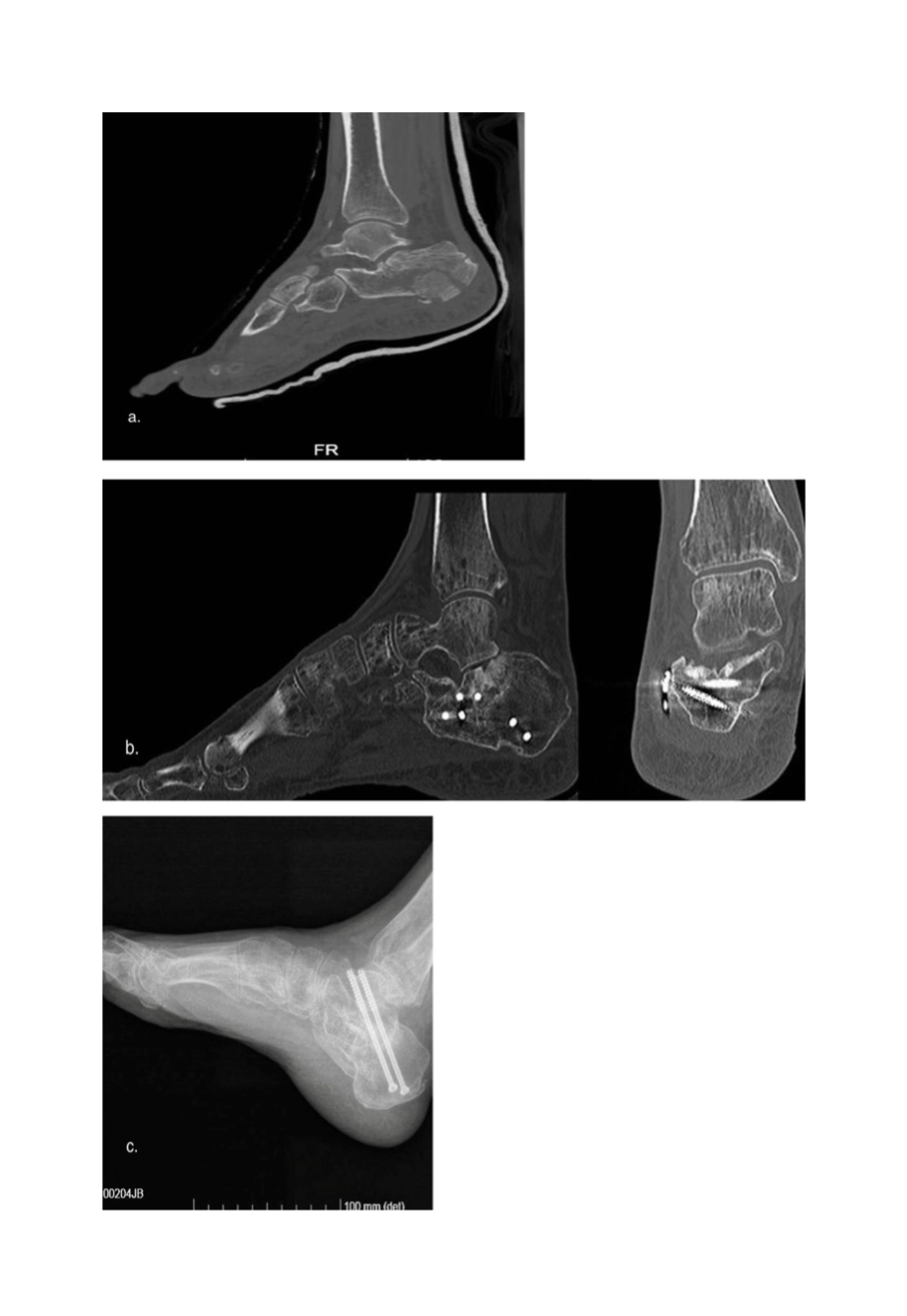
Figure 6. a, preoperative CT scan, man 56 y, (b) CT scan after 30 months, (c) post-operative (secondary subtalar arthrodesis) X-ray.
Discussion
In 1916, Cotton and Henderson18 emphasized the need for improved outcomes in treating calcaneus fractures. Since then, significant advances have been made in the management of intra-articular calcaneus fractures19. Despite the introduction of antibiotic therapy, which has helped reduce soft tissue complications, wound healing delays are still observed in 25% of patients treated for intra-articular calcaneal fractures via the standard lateral approach20.
The extensile lateral approach (ELA) is considered the gold standard for treating these fractures. It provides excellent visualization of the fracture site and facilitates accurate anatomic reduction of the articular surface. However, the ELA is associated with a high rate of complications, including fracture fragment devascularization, larger surgical exposure, wound edge necrosis or infection, and resection of the lateral calcaneal branch of the peroneal artery21,22.
Minimally invasive techniques have been developed and promoted as alternatives to the traditional ELA to minimize soft tissue complications related to the L-shaped incision. These include percutaneous fixation (for example, in tongue-type fractures according to the Essex-Lopresti classification), arthroscopically assisted fixation, and minimally invasive surgery (MIS)11,23,24. In recent years, several studies have evaluated the medium- and short-term outcomes of these approaches.
The use of MIS combined with rigid internal fixation using locking plates is now widely accepted for the treatment of most long-bone and periarticular fractures. This technique has been shown to facilitate early postoperative mobilization, accelerate rehabilitation, and promote better wound healing, thus reducing the incidence of local necrosis and infections25.
However, there are few studies26 directly comparing the outcomes of ELA and MIS combined with rigid internal fixation, and most of these studies involve small sample sizes (15-35 patients). Additionally, many studies are retrospective, with follow-up periods varying from several months to years. AOFAS scores are not included in all studies, and key factors such as time from injury to fixation, surgeon experience, incision length, and blood loss are often not reported26,27. Recent literature supports the use of MIS combined with rigid internal fixation for Sanders type II and III fractures, but fewer studies have examined its use in highly comminuted fractures (type IV in Sanders classification)28.
The sinus tarsi approach is the most frequently used limited lateral approach. In their meta-analysis, Zhang et al29 demonstrated that the sinus tarsi approach outperforms the ELA with smaller incisions, a lower incidence of wound healing complications, and a reduced postoperative VAS score. Moreover, alignment on lateral radiographs and the excellent-to-good rates according to the AOFAS score were not negatively impacted.
In 2022, Wallace et al27 described one hundred and five fractures in 100 patients treated with the sinus tarsi approach for intra-articular calcaneal fractures. The wound complication rate was 11.9%, with 1.9% requiring additional procedures.
According to many authors30-32, external fixation is typically indicated for the emergency treatment of open calcaneal fractures or closed fractures with severe soft tissue compromise. A few studies33,34 have explored percutaneous reduction and external fixation as definitive treatments for articular calcaneal fractures, irrespective of soft tissue concerns.
In 2006, Magnan et al35 described the treatment of 54 intra-articular fractures with a mini-fixator, reporting good-to-excellent outcomes in 96.7% of patients. They observed three cases of thalamic displacement due to early weight bearing. In 2024, Checa-Betegon et al33 treated 42 intra-articular calcaneus fractures with external fixator, reporting a mean postoperative AOFAS score of 79.1. Van Hoeve and Poeze36 conducted a review in 2016 evaluating outcomes after treatment with percutaneous and minimally invasive open techniques for calcaneal fractures. They found that percutaneous reduction and screw osteosynthesis, along with minimally invasive open techniques, resulted in significantly better outcomes (based on AOFAS scores and improvements in Bohler’s angle) compared to external fixation and other methods such as K-wire fixation. They also noted a higher infection rate in the external fixation group due to more frequent pin-tract infections36.
The primary goals of treatment are to restore the calcaneus’s three-dimensional structure (height, length, and width), reconstruct the subtalar joint, decompress the sub-peroneal area (avoiding peroneal conflict), reduce the calcaneocuboid surface, and align the calcaneal tuberosity in its physiological position.
In our experience, minimally invasive surgery has proven effective in achieving these objectives. Both external and internal fixation via the sinus tarsi approach have successfully restored the calcaneal height and increased the Bohler’s angle (Figure 5). According to the literature, the wound complication rate is lower with both minimally invasive techniques15,20,27,37,38.
Veltman et al39 analyzed long-term outcomes (mean follow-up 4.6 years) for 1,730 intra-articular calcaneal fractures. The average AOFAS score was 73.7 (range: 63 to 92), consistent with the findings of our study. The authors considered external fixation a good alternative for definitive treatment of intra-articular calcaneal fractures, with functional outcomes comparable to internal fixation, excluding concerns related to nursing and patient compliance.
This study has several limitations: the small sample size and the lack of randomization are the most significant.
Conclusions
MIS techniques yield results comparable to those of open reduction and internal fixation (ORIF), with the advantages of shorter waiting times, better soft tissue preservation, and reduced complication rates23-25. Both internal and external fixation provide excellent outcomes for the treatment of Sanders type II and III fractures. The choice between the two approaches should be guided by the surgeon’s experience and the specific clinical scenario.
Conflict of Interest
The authors declare that they have no conflict of interest to disclose.
Authors’ Contributions
M.B. and A.P. participated in the drafting and critical revision of the manuscript. L.P. contributed extensively to the study’s methodology development and was instrumental in the acquisition of data. Additionally, M.B. played a key role in interpreting the data and provided substantial input in the writing and editing of the manuscript. L.P. was deeply involved in data analysis and interpretation. A.P. and G.Z. contributed significantly to the drafting of the manuscript, particularly in the discussion and conclusion sections.
Ethics Approval and Informed Consent
The study protocol received approval from the local Ethics Committee (Val Padana 39/2018 – June 19, 2019). All patients signed an informed consent to allow the study and the publication of the results anonymously.
Availability of Data and Materials
Data are available on reasonable request by the author L.P.
AI Disclosure
No AI was used.
Funding
None.
ORCID ID
MB: 0000-0001-6766-3720
References
- Atkins RM, Allen PE, Livingstone JA. Demographic features of intra-articular fractures of the calcaneum. Foot Ankle Surg 2000; 7: 77-84.
- Sharr PJ, Mangupli MM, Winson IG, Buckley RE. Current management options for displaced intra-articular calcaneal fractures: Non-operative, ORIF, minimally invasive reduction and fixation, or primary ORIF and subtalar arthrodesis. A contemporary review. Foot Ankle Surg 2015; 22: 1-8.
- Buckley R, Tough S, McCormack R, Pate G, Leighton R, Petrie D, Galpin R. Operative compared with non-operative treatment of displaced intra-articular calcaneus fractures: a prospective, randomized, controlled multi-center trial. JBJS Am 2002; 84: 1733-1744.
- Csizy M, Buckley R, Tough S, Leighton R, Smith J, McCormack R, Pate G, Petrie D, Galpin R. Displaced intra-articular calcaneal fractures: variables predicting late subtalar fusion. J Orthop Trauma 2003; 2: 106-112.
- Barla J, Buckley R, Tough S, Pate G, Leighton R, Petrie D, Galpin R, Canadian Orthopaedic Trauma Society. Displaced intra-articular calcaneal fractures: long-term outcome in women. Foot Ankle Int 2004; 25: 853-856.
- Ibrahim T, Rowsell M, Rennie W, Brown AR, Taylor GJ, Gregg PJ. Displaced intra-articular calcaneal fractures: 15-year follow-up of a randomised controlled trial of conservative versus operative treatment. Injury 2007; 38: 848-855.
- Leung KS, Yuen KM, Chan WS. Operative treatment of displaced intra-articular fractures of the calcaneum. Medium-term results. J Bone Joint Surg Br 1993; 75: 196-201.
- Crosby LA, Fitzgibbons T. Computerized tomography scanning of acute intra-articular fractures of the calcaneus. A new classification system. JBJS Am 1990; 72: 852-859.
- Clare MP, Crawford WS. Managing complications of calcaneus fractures. Foot Ankle Clin 2017; 22: 105-116.
- Howard JL, Buckley R, McCormack R, Pate G, Leighton R, Petrie D, Galpin R. Complications following management of displaced intra-articular calcaneal fractures: a prospective randomized trial comparing open reduction internal fixation with nonoperative management. J Orthop Trauma 2003; 17: 241-249.
- Magnan B, Bondi M, Mezzari S, Bonetti I, Samaila E. Minimally Invasive Surgery of the Forefoot: Current Concept Review. Int J Clin Med 2013; 4: 11-19.
- Brauner CA, Manns BJ, Ko M, Donaldson C, Buckley R. An economic evaluation of operative compared with non-operative management of displaced intra-articular calcaneal fractures. J Bone Joint Surg Am 2005; 12: 2741-2749.
- MacKenzie EJ, Morris JA Jr, Jurkovich GJ, Yasui Y, Cushing BM, Burgess AR, DeLateur BJ, McAndrew MP, Swiontkowski MF. Return to work following injury: the role of economic, social, and job-related factors. Am J Public Healt 1998; 88: 1630-1637
- Van Tetering EA, Buckley RE. Functional outcome (SF-36) of patients with displaced calcaneal fractures compared to SF-36 normative data. Foot Ankle Int 2004; 25: 733-738.
- Sanders R, Fortin P, DiPasquale T, Walling A. Operative treatment in 120 displaced intraarticular calcaneal fractures: results using a prognostic computed tomography scan classification. Clin Orthop 1993; 290: 87-95.
- Bohler L. Diagnosis, Pathology and treatment of fractures of the os calcis. J Bone Joint Surg 1931; 13: 75-89.
- Gissane W. Discussion on fractures of the os calcis. Proceedings of the British Orthopaedic Association. J Bone Joint Surg Am 1947; 29: 254-255.
- Cotton FJ, Henderson FF. Results of fractures of the os calcis. Amer J Orthop Surg 1916; s2-14: 290-298.
- Piotto L, Bondi M, Pizzoli A. La frattura dell’amante: breve storia del trattamento delle fratture di calcagno. GIOT 2019; 45: 120-123.
- Benirschke SK, Kramer PA. Wound healing complications in closed and open calcaneal fractures. J Orthop Trauma 2004; 18: 1-6.
- Bergin PF, Psaradellis T, Krosin MT, Wild JR, Stone MB, Musapatika D, Weber TG. Inpatient soft tissue protocol and wound complications in calcaneus fractures. Foot Ankle Int 2012; 33: 492-497
- Agren PH, Mukka S, Tullberg T, Wretenberg P, Sayed-Noor AS. Factors affecting long-term treatment results of displaced intra-articular calcaneal fractures: a post hoc analysis of a prospective, randomized, controlled, multi-center trial. J Orthop Trauma 2014; 28: 564-568
- Giannini S, Cadossi M, Mosca M, Tedesco G, Sambri A, Terrando S, Mazzotti A. Minimally invasive treatment of calcaneal fractures: a review of the literature and our experience. Injury 2016; 47: 138-146.
- Hollawell S, Coleman M, Yancovitz S. Arthroscopy of Foot and Ankle: Subtalar Joint Arthroscopy in Intra-articular Calcaneal Fractures. Clin Podiatr Med Surg 2023; 40: 519-528.
- Lappalainen TA, Noponen NA, Kaarela OI, Klemola TM, Ohtonen PP, Leppilahti JI. Postoperative complications after displaced intra-articular calcaneal fracture operations. Foot Ankle Surg 2024; 30: 319-324.
- Wu Z, Su Y, Chen W, Zhang Q, Liu Y, Li M, Wang H, Zhang Y. Functional outcome of displaced intra-articular calcaneal fractures: a comparison between open reduction/internal fixation and a minimally invasive approach featured an anatomical plate and compression bolts. J Trauma Acute Care Surg 2012; 73: 743-751.
- Wallace B, Chhabra A, Narayanan A, O’Neill D, Xi Y, Van Pelt M, Wukich DK, Liu G, Sanders D, Lalli T. Low Risk of Wound Complications With Sinus Tarsi Approach for Treatment of Calcaneus Fractures. J Foot Ankle Surg 2022; 61: 771-775.
- Khazen G, Rassi CK. Sinus Tarsi Approach for Calcaneal Fractures: The New Gold Standard? Foot Ankle Clin 2020; 25: 667-681.
- Zhang F, Tian H, Li S, Liu B, Dong T, Zhu Y, Zhang Y. Meta-analysis of two surgical approaches for calcaneal fractures: sinus tarsi versus extensile lateral approach. ANZ J Surg 2017; 87: 126-131.
- Besch L, Waldschmidt JS, Daniels-Wredenhagen M, Varoga D, Mueller M, Hilgert RE, Mathiak G, Oestern S, Lippross S, Seekamp A. The treatment of intra-articular calcaneus fractures with severe soft tissue damage with a hinged external fixator or internal stabilization: long-term results. J Foot Ankle Surg 2010; 49: 8-15.
- Hammond AW, Crist BD. Percutaneous treatment of high-risk patients with intra-articular calcaneus fractures: a case series. Injury 2013; 44: 1483-1485.
- Farrell BM, Lin CA, Moon CN. Temporising external fixation of calcaneus fractures prior to definitive plate fixation: a case series. Injury 2015; 46: 19-22.
- Checa-Betegón P, Valle-Cruz J, Llanos-Sanz S, Miguel-Miguel C, Sánchez-Del-Saz J, García-Coiradas J. External fixation in intra-articular fractures of the calcaneus: Is it a valid option as definitive treatment? Eur J Orthop Surg Traumatol 2024; 34: 201-208.
- Wang J, Qin S, Wang T, Liu J, Wang Z. Comparison of the Curative Effect of Percutaneous Reduction with Plastic Calcaneal Forceps Combined with Medial External Fixation in the Treatment of Intra-Articular Calcaneal Fractures. Orthop Surg 2021; 13: 2344-2354.
- Magnan B, Bortolazzi R, Marangon A, Marino M, Dall’Oca C, Bartolozzi P. External fixation for displaced intra-articular fractures of the calcaneum. J Bone Joint Surg Br 2006; 88: 1474-1479.
- Van Hoeve S, Poeze M. Outcome of Minimally Invasive Open and Percutaneous Techniques for Repair of Calcaneal Fractures: A Systematic Review. J Foot Ankle Surg 2016; 55: 1256-1263.
- Folk JW, Starr AJ, Early JS. Early wound complications of operative treatment of calcaneus fractures: analysis of 190 fractures. J Orthop Trauma 1999; 13: 369-372.
- Lim EV, Leung JP. Complications of intraarticular calcaneal fractures. Clin Orthop 2001; 391: 7-16.
- Veltman ES, Doomberg JN, Stufkens SA, Luitse JS, van den Bekerom MP. Long-term outcomes of 1,730 calcaneal fractures: systematic review of the literature. J Foot Ankle Surg 2013; 52: 486-490.
To cite this article
Minimally invasive treatment of calcaneus fracture
JOINTS 2025;
3: e1651
DOI: 10.26355/joints_20259_1651
Publication History
Submission date: 29 Jul 2024
Revised on: 16 Sep 2024
Accepted on: 05 Sep 2025
Published online: 18 Sep 2025