JOINTS 2025;
3: e1649
DOI: 10.26355/joints_20259_1649
Use of stem with metaphyseal sleeves in revision total knee arthroplasty: is it worth the hassle? a systematic review
Topic: Knee
Category: Systematic Review
Abstract
OBJECTIVE: Revision total knee arthroplasty (rTKA) is a technically demanding procedure due to the variability of surgical tools and the lack of standardized protocols. Achieving long-term stable fixation is especially challenging in cases with compromised bone stock. This systematic review evaluates the feasibility of using metaphyseal sleeves without stems as a fixation method in rTKA.
MATERIALS AND METHODS: We conducted a systematic review of the literature, including clinical studies and biomechanical analyses focusing on the use of metaphyseal sleeves without stems in rTKA. A total of nine studies were selected: five clinical studies (two prospective and three retrospective) and four biomechanical or finite-element analyses. Outcomes assessed included clinical results, radiological findings, complication rates, failure rates, and biomechanical performance.
RESULTS: Stemless metaphyseal sleeves demonstrated promising clinical and radiological outcomes. The overall failure rate due to aseptic loosening was 3%. Proper fixation in zones 1 and 2 was achievable with metaphyseal sleeves alone, while additional stems were necessary when stability in zone 3 was compromised. Biomechanical analyses indicated that smaller sleeves enhanced both rotational and axial stability.
CONCLUSIONS: The use of metaphyseal sleeves without stems appears to be a viable fixation option in rTKA, provided that adequate preoperative planning and intraoperative evaluation are performed. These findings suggest that, under appropriate conditions, stemless fixation can achieve reliable stability, potentially reducing the morbidity associated with stem use. However, limitations such as small sample sizes and short follow-up periods in the reviewed studies highlight the need for caution when generalizing these results.
Introduction
Revision total knee arthroplasty (rTKA) poses significant challenges in achieving stable, long-term fixation, particularly when residual bone stock is compromised1. The integrity of the metaphyseal region is crucial for attaining optimal stability in a revision construct. This area, due to its rich vascularization and reduced susceptibility to surgical damage compared to the epiphyseal bone, facilitates cement interdigitation and implant osteointegration, contributing to superior initial fixation and prolonged implant survival2. In cases with substantial bone defects, two commonly adopted global approaches leverage these properties: the use of cones and metaphyseal sleeves3. These constructs differ significantly. Cones, which serve as fillers, are used to fill defect sizes and enhance the fixation of cemented implants without structural integration with other components. In contrast, metaphyseal sleeves are integrated parts of the implant, providing primary and direct fixation while aiding in load transfer from the revision components to the metaphyseal region. Additionally, metaphyseal sleeves offer the potential for bony biologic fixation, improving rotational stability and protecting epiphyseal fixation. Compared to fluted cylindrical stems, metaphyseal sleeves are more effective in achieving these objectives4. Clinicians typically use stems initially to stabilize sleeves (Figure 1), but there is an increasing trend toward using sleeves without stems (Figure 2). However, studies on this approach are limited by small sample sizes, lack of control groups, and short follow-up periods. Importantly, there is currently no consensus on the necessity of using stems with metaphyseal sleeves. This systematic review aims to summarize the contemporary literature to determine whether using metaphyseal sleeves without stems in rTKA is a valuable option.
Figure 1. Stemmed sleeve configuration in revision total knee arthroplasty.
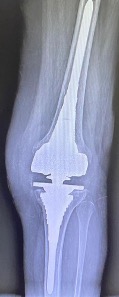
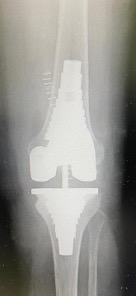
Figure 2. Stemless sleeve configuration in revision total knee arthroplasty.
Materials and Methods
An electronic search was conducted on May 1st, 2024, using the PubMed (MEDLINE) database to investigate the use of sleeves without stems in revision total knee arthroplasty (rTKA). As this was a systematic review, PRISMA guidelines were applied in the selection and synthesis of the literature. This search was conducted with multiple strings, including “metaphyseal AND sleeves” (122 studies) and “sleeve AND stem AND knee” (45 studies), and involved reviewing the titles and abstracts of each study. Out of these, we identified 11 relevant studies that reported clinical results, radiological outcomes, complications, and failure rates, as well as those that conducted finite-element analysis on rTKAs with metaphyseal sleeves without stems.
Articles not written in English, those reporting an inaccurate number of stemless sleeves used, or those that included too few stemless sleeves in comparison to the total cohort evaluated were excluded. Additionally, literature reviews and letters to the editor were also excluded. The references for each of the included papers were reviewed to identify any potential studies that may have been missed.
Data Extraction
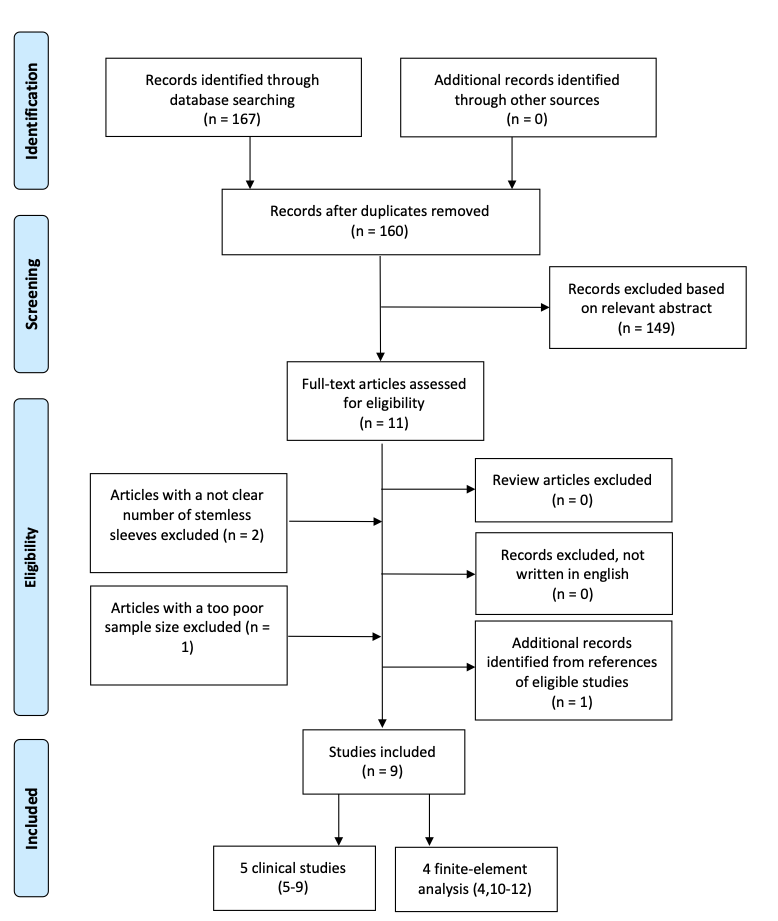
Extracted data included years of follow-up, indications for revision, preoperative Anderson Orthopedic Research Institute (AORI) classification type (Table 1), knee clinical outcomes score, radiological findings, and reasons and rates for failures (Table 2 and Table 3). All data were compiled in a Microsoft Excel spreadsheet (2021; Microsoft Corporation, Redmond, WA, USA). The overall search process (Figure 3) produced 9 studies4-12 for final inclusion in our analysis: 5 clinical studies5-9, of which 2 were prospective studies and 3 were retrospective studies (Table 2), and 4 biomechanical studies and finite-element analysis4,10-12.
Table 1. Anderson Orthopedic Research Institute (AORI) classification.
| Type | Severity of bone defects in tibia (T) and femur (F) |
| 1 (T1 and F1) | Minor bone defect without compromising the stability of a component |
| 2A (T2A and F2A) | Metaphyseal bone damage and cancellous bone loss in one femoral condyle/tibial plateau requiring reconstruction to maintain implant stability |
| 2B (T2B and F2B) | Metaphyseal bone damage and cancellous bone loss in both femoral condyles/tibial plateau |
| 3 (T3 and F3) | Significant cancellous metaphyseal bone loss compromising a major portion of either femoral condyles or tibial plateau, occasionally associated with patellar tendon or collateral ligament detachment |
Table 2. List of included studies.
| Study | Year of publication | Type of study | Number of patients and implants | Mean follow-up | AORI (number of patients) | Indication (cases) | Implant (DePuy Orthopedics, Warsaw, IN) |
| Graichen et al9 | 2015 | Prospective study | 121 patients, 119 tibial sleeves and 74 femoral sleeves (2 cases of stemless fixation of the tibia and 49 of the femur) | 3.6 years | Femur: Type IIB (93), Type III (28). Tibia: Type II (114), Type III (7) | Instability (41), malalignment (24) and loosening (23), polyethylene wear (15), trauma (4), stiffness (9), implant failure (3) and pain (2). In some cases, more than one problem was identified. | The Press-Fit Condylar (P.F.C.) Sigma mobile bearing Revision Knee. In 77 patients a posterior stabilized insert, in 27 a TC3 insert (varus-valgus constrained), and in 17 a rotating hinge was implanted. |
| Bugler et al6 | 2015 | Retrospective study | 35 patients. Sleeves configuration: femoral and tibial in 14 (69%), only tibial in 10 (28%) or femoral 1 (3%); stem in 21 (60%) of the tibial and 12 (34%) of the femoral. | 3.25 years | Type I: (20), Type II: (13), Type III: (2) | Aseptic loosening (45%), polyethylene wear (26%), malalignment (17%), instability (6%), unexplained pain (6%). | Hinged S-ROM Noiles knee system. |
| Gøttsche et al7 | 2016 | Retrospective study | 63 patients | > 2 years | Femur: Type I (7%), Type IIA (33%), Type IIB (56%), Type III (5%). Tibia: Type I (9%), Type IIA (9%), Type IIB (63%), Type III (19%). | Aseptic loosening (32), pain (18), infection (16), stiff knee (2), instability (1), fracture (1), polyethylene wear (1). | The Press-Fit Condylar (P.F.C.) Sigma Rotating Platform TC3 Revision Knee. |
| Scior et al8 | 2019 | Prospective study | 85 patients, 109 stemless metaphyseal sleeves (81 femoral, 28 tibial) | 4.8 years | Type I or type IIA | Aseptic loosening (34, 36.6%), instability (28, 30.1%), malalignment (18, 19.4%), stiffness (10, 11.8%). In some cases, more than one problem was identified. | The Press-Fit Condylar (P.F.C.) Sigma Rotating Platform TC3 Revision Knee. |
| Stefani et al5 | 2019 | Retrospective study | 121 knees, 44 in the group without stems and 77 in the group with stems | 5.25 years for the stemless group, 7.4 years for the stems group | Type I in 24 femur and 25 tibia, Type IIA-IIB in 98 femur and 102 tibia, Type III in 21 femur and 16 tibia | Aseptic loosening 61 (42%), periprosthetic joint infection 46 (32%), instability 11 (8%), fracture 6 (4%), poli wear 4 (3%), arthrofibrosis 4 (3%), and other causes 11 (8%). | SIGMA TC3 revision implant with a posterior stabilized insert and a TC3 (varus-valgus constrained) insert. |
Anderson Orthopedic Research Institute (AORI).
Table 3. Failure rate and complications.
| Study | Mean BMI | Mean age (years) | Exclusion criteria | Final alignment | Survival rate of stemless sleeves from aseptic loosening | Causes of failure |
| Graichen et al9 | 32.9 ± 6.9 | 74 ± 9 | < 70% sleeve-bone contact | 98.4 % MA ± 3° | 120/121 tibial (99.2%) | 1/121 tibial (0.8%) and 3/121 femoral sleeves (2.7%) aseptic loosening (rotating hinge implant) |
| 118/121 femoral (97.3%) | 4 (3.3%) infection | |||||
| 238/242 (98.3%) overall | 5 (4.1%) biomechanical reasons: 3 ligament instability, 1 malalignment, 1 extensor mechanism failure | |||||
| 3/121 radiolucent lines (2 femoral, 1 tibial) | ||||||
| 2 failures of the implant (broken at the junction between stem and sleeve) | ||||||
| Bugler et al6 | 30.2 (20-42) | 72 (55-86) | Uncontained defects in zone 1, 2 or 3 | Not reported | 35/35 (100%) | 3/35 (8.6%) patients with patellofemoral symptoms necessitating patellofemoral arthroplasty |
| No radiolucent lines | ||||||
| Gøttsche et al7 | Demographic data not reported | Demographic data not reported | No criteria based on type of defect | 49% inside optimal range (2.4-7.2° valgus), 51% outside range | 69/71 (97.2%)¥ | 2/71 (2.8%) aseptic loosening |
| 7/63 (11.1%) radiolucent lines | 1/71 (1.4%) infection | |||||
| 1/71 (1.4%) instability | ||||||
| 1/71 (1.4%) pain without loosening | ||||||
| Scior et al8 | Demographic data not reported | Demographic data not reported | AORI type IIB or III | 100% MA ± 3° | 96% tibia (27/28) | 1/28 (3.6%) tibial aseptic loosening |
| 100% femur (81/81) | 4/28 (4.7%) infection | |||||
| 99% (108/109) overall | 2/28 (2.4%) patella baja | |||||
| 1/28 radiolucent lines (tibial) | 2 (2.4%) instability | |||||
| 1 (1.2%) periprosthetic femur fracture | ||||||
| Stefani et al5 | Not reported | 73 | < 70% sleeve-bone contact or poor bone quality | Not reported | 121/121 (100%) | 3/144 infection*§ |
| 8/121 with radiolucent lines (3 femoral, 5 tibial), 6 of which without symptoms* | 1/144 instability*§ | |||||
| 1/144 periprosthetic femoral fracture*§ | ||||||
| 1/144 patello-femoral symptoms*§ |
(¥) The authors only included the 63 out of 71 patients who at least answered the questionnaire and the subjective part of the AKSS; (*) The authors did not specify whether these complications happened in the stemless or in the stemmed group; (§) Excluded from the study since the failure was not related to sleeves.
Anderson Orthopedic Research Institute (AORI); Body Mass Index (BMI); Mechanical Alignment (MA); American Knee Society Score (AKSS).
Results
Clinical Outcomes
We identified several clinical scoring systems across the five clinical studies5-9 (Table 4). Graichen et al9 focused on assessing the effectiveness of rTKA in 121 patients who received 119 tibial sleeves and 74 femoral sleeves, including 2 cases of stemless tibial fixation and 49 cases of stemless femoral fixation, measuring the range of motion (ROM) and the American Knee Society Score (AKSS). The results showed a significant improvement in the mean ROM, from 89° ± 6° to 114° ± 4°, and the mean AKSS, from 88 ± 18 to 147 ± 23 (p < 0.01). The mean AKS functional score also showed improvement, from 52 ± 18.9 to 68.8 ± 23.3 (p < 0.01). The study found no significant difference between the stemless and stemmed groups. A retrospective analysis by Bugler et al6 included 35 cases of rTKA, with 14 cases involving both femoral and tibial sleeves (69%), 10 cases involving only tibial sleeves (28%), and 1 case involving only a femoral sleeve (3%), 21 (60%) of the tibial prostheses and 12 (34%) of the femoral prostheses included stems, while the remaining sleeves were stemless. The post-operative Knee Society Score (KSS) was reported as good in 20% and excellent in 63% of the patients, and 63% of the patients expressed good satisfaction scores (rated 8 out of 10 or higher). Patients achieved full extension (83%), with a mean flexion angle of 100 degrees, ranging from 70 to 130 degrees. The authors did not report differences between the stemless and stemmed groups. Gøttsche et al7 reported outcomes of 63 patients who underwent rTKA using sleeves without stem augmentation. They observed a mean AKSS improvement from 62.7 (54.7-70.8) to 109.6 (98.1-121.2) (p < 0.0001) and a mean postoperative Oxford Knee Score (OKS) of 27.9 (24.7-31.0). A statistically significant increase in pain scores with increasing functional limitations was noted (p = 0.028). Additionally, they reported that 30% of the patients were dissatisfied, while 21% were partially satisfied. Scior et al8 evaluated 85 rTKAs with 109 stemless sleeves (81 femoral, 28 tibial). They found an average improvement in ROM from 97.7° to 114.1°, as well as increases in the KSS and Functional Knee Score from 88.8 to 159.3 and from 38.2 to 74.1, respectively. The OKS also showed an improvement of 18.6 points, from 21.2 to 39.8. In a more recent retrospective study, Stefani et al5 investigated 121 rTKA procedures in which metaphyseal sleeves were utilized on either the tibial or femoral side, or both, 44 of which were without stems, and 77 with stems. The authors reported a statistically significant increase in the mean KSS score from 34 to 81 (39 to 81 in the stemless group) (p < 0.01), and a significant improvement in the mean Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) score from 82% to 39% (76% to 37% in the stemless group) (p < 0.01). However, no significant differences were found between the two groups. While it might seem inconsequential to assess clinical scores for evaluating the effectiveness of a mechanically oriented system, it remains valuable to observe the absence of statistically significant variances. The notion of avoiding shaft invasion to enhance fixation is driven by concerns regarding “stem end pain”. Intriguingly, the gathered studies consistently indicate that, despite the well-intentioned approach, the presence or absence of the stem does not impact post-operative pain scores.
| Study | Number of patients | Range of motion (ROM) | American Knee Society Score (AKSS) | Knee Society Score (KSS)
|
Post-operative Oxford Knee Score (OKS) | Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) | Differences between stemless and stemmed groups |
| Graichen et al9 | 121 patients, 119 tibial sleeves and 74 femoral sleeves (2 cases of stemless fixation of the tibia and 49 of the femur) | From 89° ± 6° to 114° ± 4° | From 88 ± 18 to 147 ± 23 | – | – | – | NO |
| Bugler et al6 | 35 patients. Sleeves configuration: femoral and tibial in 14 (69%), only tibial in 10 (28%) or femoral 1 (3%); stem in 21 (60%) of the tibial and 12 (34%) of the femoral. | – | – | 20% good, 63% excellent (post-operative) | – | – | NO |
| Gøttsche et al7 | 63 patients, 63 stemless metaphyseal sleeves | – | From 62.7 to 109.6 | – | 27.9 | – | – |
| Scior et al8 | 85 patients, 109 stemless metaphyseal sleeves (81 femoral, 28 tibial) | – | – | From 88.8 to 159 | – | – | – |
| Stefani et al5 | 121 knees, 44 stemless metaphyseal sleeves and 77 stemmed metaphyseal sleeves | – | – | From 34 to 81 stemmed group; from 39 to 81 stemless group | – | From 82% to 39% stemmed group; 76% to 37% stemless group | YES (p < 0.01) |
Radiographic Outcomes
The radiographic outcomes across the studies included provided encouraging results, demonstrating favorable osteointegration and alignment in the majority of cases, with only a small number of patients experiencing radiolucent lines or other complications. Graichen et al9 found that the majority of the sleeves (96.4%) exhibited excellent osteointegration in both planes. Only seven patients showed radiolucent lines around the coated area of the sleeves, with five cases involving the femoral side and two cases involving the tibial side. Among these seven patients, three remained asymptomatic. The restoration of leg axis was achieved in almost all cases within a 3° corridor (98.4%), and the mean leg axis shifted from 2.1° ± 2.2° varus preoperatively to 0.6° ± 0.3° varus postoperatively. Bugler et al6 reported no evidence of osteolysis or loosening of the femoral or tibial prostheses. Gøttsche et al7 observed radiolucent lines around the prosthesis in only seven patients (11%), with a cortical reaction seen in five patients (8%). Additionally, they noted optimal alignment in 51% of cases, with a mean tibiofemoral alignment of 6° of valgus. Scior et al8 also observed excellent osteointegration of sleeves in both planes in most patients (99.1%). Moreover, they reported that the mean long leg mechanical axis changed from 3.1° ± 2.5° of varus preoperatively to 1.4° ± 0.3° of valgus postoperatively (p < 0.01), with a joint line shift of approximately 2.8 mm compared to the preoperative assessment. Finally, radiological findings from Stefani et al5 showed good overall osteointegration of prosthetic implants. Only eight radiolucent lines (three femoral, five tibial) were observed around the sleeves, with only two of those having clinical correlations.
Biomechanical Results from Finite-Element Studies
The initial press-fit of the implant achieved during surgery is crucial for determining long-term outcomes13. However, natural bone remodeling over time can weaken the local contact areas between the bone and implant14. Large metal components can alter the strain-stress behavior at the bone-implant interface. To better understand and predict the biomechanical behavior of stemless metaphyseal sleeves in rTKA in the medium to long term, several authors4,10-12 have conducted in vitro analyses to evaluate this implant fixation technique (Table 5).
Fonseca et al10 performed an experimental and finite-element analysis using five synthetic femurs to measure cortex strain behavior and implant-cortex micromotions for three types of prosthetic implants in rTKA: femoral-component-only, stemless sleeve, and stemmed sleeve. Their study revealed that a stem is not necessary for achieving high stability in the initial fixation of a sleeve-bone construct. While a stem may affect the strain behavior of cancellous bone, its impact is secondary. Both techniques showed acceptable micromotions ranging from 50 to 150 microns, promoting bone ingrowth. This finding aligns with Wolff’s law, stating that bone tissue adapts and remodels in response to the loading it experiences. Mechanical stimuli significantly impact bone ingrowth, alongside biological and biomechanical processes. Higher loading stimulates osteoblasts to strengthen bone, while lower loading leads to osteoclasts reducing bone tissue14-16. Research has shown that extensive relative motions exceeding 150 microns can disrupt established bony bridges, leading to fibrous connective tissue formation at the implant-bone interface, complicating osseointegration17-19. These processes can result in aseptic loosening and implant failure20.
Table 5. (S+S) stemmed sleeve.
| Study | Finding A | Finding B | Finding C |
| Fonseca et al10 | S+S is not necessary to achieve a high-level initial fixation of a sleeve-bone construct | S+S may reduce surrounding cancellous bone strain, but its effect appears to be secondary | |
| Frehill and Crocombe12 | S+S may reduce stress concentrations
|
S+S promotes more resorption in the cancellous bone near the sleeve | Smaller sleeves provided better rotational and axial stability with lower surrounding stress concentrations |
| Awadalla et al11 | S+S did not significantly improve primary fixation | S+S resulted in distal load transfer to the diaphysis and in a reduction in strain in the surrounding area | |
| Nadorf et al4 | A small canal filling stem can improve initial fixation
|
The increased risk of proximal stress shielding in S+S constructs outweighs the benefits of better initial fixation |
Structurally, a diaphyseal femoral stem in combination with a metaphyseal sleeve may not be necessary in rTKA, particularly where stem usage is impractical. Incorporating a diaphyseal stem increases the risk of cortical bone resorption compared to the stemless sleeve approach. Frehill and Crocombe12 assessed the effectiveness of using stems with cementless metaphyseal sleeves for treating AORI Type III bone defects in rTKA. Their findings showed that a press-fit stem could reduce stress concentrations but also promote more resorption in the cancellous bone surrounding the sleeve. Consequently, they did not recommend using stems to treat AORI Type III bone defects with metaphyseal sleeves. Additionally, the study compared different sizes of metaphyseal sleeves and concluded that smaller sleeves provided better rotational and axial stability, resulting in lower stress concentrations in the proximal cancellous bone and better preservation of the metaphyseal bone stock. Awadalla et al11 used computed tomography (CT) scans to create finite element models to investigate proximal tibial bone strain distribution and primary stability of a cementless rotating platform tibial tray with a sleeve, with or without a stem, in an AORI Type IIB defect. They analyzed data from applying joint contact forces mimicking level gait, stair descent, and squat movements. The results showed that stemless sleeved implants exhibited satisfactory primary stability, with micromotions below 50 microns and strains well below the bone yield point under various loading conditions. The addition of a stem did not significantly enhance primary stability when the sleeve already provided adequate mechanical stability but led to distal load transfer to the diaphysis and reduced strain in the bone adjacent to the implant. Nadorf et al4 investigated the use of stems in AORI Type I bone defects and the benefits of different stem options combined with large metaphyseal sleeves in a modular tibial revision knee system. Their tests applying axial and varus-valgus torques showed that a short (one size thinner but still canal-filling) or flexible stem provided better initial stability and supported metaphyseal fixation while allowing bending similar to intact bone. However, there was an increased risk of proximal stress shielding in constructs with incorporated stems, outweighing the benefits of better initial fixation.
Complications and Failure Rate
The analysis of data from five clinical studies5-9 underscores the favorable outcomes associated with the use of stemless metaphyseal sleeves in revision total knee arthroplasty (rTKA). These outcomes include low rates of septic and aseptic loosening, a reduced incidence of intraoperative fractures, and satisfactory short-term follow-up results. Graichen et al9 reported 14 revisions during a mean follow-up of 3.6 years, accounting for 11.4% of cases. Among these, four revisions (3.3%) were attributed to periprosthetic joint infection (PJI). Aseptic revisions, comprising 5 cases (4.1%), were primarily due to biomechanical complications: ligament instability (three cases), malalignment (one case), and extensor mechanism failure (one case). Additionally, implant failure at the junction between the stem and sleeve occurred in two patients. The overall aseptic survival rate for metaphyseal sleeves was 98.3% at 3.6 years, with no significant differences between stemmed and stemless groups. Bugler et al6 documented two cases of wound infection, one case of knee instability, three cases of patellofemoral symptoms, and one case of late femoral condyle fracture. Notably, no early loosening was observed, and none of the patients required re-revision. The authors reported no significant differences between the outcomes of stemmed and stemless groups. In the study by Gøttsche et al7, two cases of aseptic loosening (2.8%) were identified, while Scior et al8 noted a total of 4 patients (4.7%) with PJI, 2 patients (2.4%) with stiffness due to patella baja, 2 patients (2.4%) with knee instability, 1 patient (1.2%) with a periprosthetic femur fracture, and 1 patient (1.2%) with tibial loosening. The overall survival rate was 88.2%, with an aseptic survival rate of 99% at five years. No complications or implant failures were reported in the study by Stefani et al5. In summary, across the five included studies encompassing a total of 214 stemless sleeves in rTKA, only seven cases (3%) of aseptic loosening were reported at the latest follow-up. While these results are promising, they should be interpreted with caution due to potential numerical biases and the relatively small patient sample sizes and limited follow-up periods. Nonetheless, current evidence suggests no significant differences in clinical outcomes between the use of stemmed and stemless sleeves in rTKA.
Discussion
The most important finding highlighted by this systematic review is that stemless metaphyseal sleeves demonstrated promising results, with an overall failure rate of only 3% due to aseptic loosening.
In planning rTKA, Morgan-Jones et al1 introduced a zonal fixation approach based on the identification of three crucial anatomical zones for fixation in the distal femur and proximal tibia: zone 1 (joint surface or epiphysis), zone 2 (metaphysis), and zone 3 (diaphysis), allowing for pre-operative planning and providing an understanding of where secure fixation can be achieved. It is recommended that implant fixation be achieved in at least two of these zones. In most cases of rTKA, zone 1 is frequently compromised, leading many surgeons to use stems to improve the stability and fixation of prosthetic components. However, metaphyseal sleeves have emerged as a popular option for patients with severe metaphyseal bone defects. The sleeves can provide reliable fixation in zones 1 and 2; moreover, smaller sleeves were found to offer better rotational and axial stability. Haidukewych et al2 suggest that the use of sleeves or cones, rather than stems, may provide the necessary stability by allowing ingrowth of both components. Despite metaphyseal sleeves being initially used in conjunction with stems, the specific advantages and contributions they offer are not thoroughly understood. Currently, there is no consensus on whether metaphyseal sleeves should be employed without stems. The introduction of this fixation method in rTKA was initially motivated by concerns about “end-of-stem pain” and malalignment in bowed tibia and femur21. An 11% incidence of “end-of-stem pain” was reported for femoral stems and 14% for tibial stems in a study conducted by Barrack et al21, which included 66 femur and 50 tibia cases. Their study also revealed a close correlation between this pain and patient satisfaction, as reported by Gøttsche et al7. They found no significant difference in functional scores and satisfaction, suggesting that patients can tolerate functional disability better than pain. In our review, we found that regardless of whether the stem is present or absent, there is no substantial impact on postoperative pain scores, despite the well-meaning intentions. Although sleeves are designed to achieve fixation mainly in the metaphyseal area, with the components averaging approximately 70 mm in length, the commonly observed phenomenon of “end-of-stem pain” may persist. Another hypothesis to consider is that the high percentage of patients experiencing pain could be attributed to the large number of knees with suboptimal alignment, which is a typical issue associated with the use of stems. Gobba et al22 found that in revision implants, the use of a 120 mm tibial stem could cause the tibial tray to be positioned excessively valgus, while using a 200 mm tibial stem could force the tray into a posteromedial position. Additionally, Stefani et al5 suggested that the use of a stem in the femur could complicate flexion of the femoral component, even with available offset stems that are difficult to use. Without a stem, achieving up to 7 degrees of flexion is feasible, filling a flexion gap of up to 5 mm without causing any extension deficit. By employing metaphyseal fixation, as seen in sleeves, it becomes feasible to make alignment adjustments and prevent deformities in the same-side limbs or hardware, which would not be achievable through diaphyseal engagement. These advantages hold true when the procedure is performed by a skilled surgeon. Without the guidance provided by the diaphyseal guide, the available references for ensuring accurate alignment of the components diminish, posing a significant risk in rTKA. An additional aspect worth considering is the biomechanical perspective: the utilization of sleeves, rather than stems, places the implant fixation in closer proximity to the joint line. This proximity aids in achieving a more favorable soft tissue balance23 and permits the use of untethered implants24. This makes sleeves without stems a promising option that simplifies bone preparation, reduces operating time, and lowers revision costs.
Conclusions
While higher-quality studies than those included in this systematic review may offer additional insights, the use of sleeves without stems appears to be a promising treatment option. This approach simplifies bone preparation, reduces operative duration, and lowers revision costs. However, further research involving larger patient cohorts is necessary to draw definitive conclusions.
Ethics Approval
Not applicable due to the nature of the study.
Informed Consent
All images used were taken from patients who underwent surgery by the authors, and who gave informed consent for their clinical and radiographic data to be used for scientific diffusion and research purposes. The images are fully anonymous, and no personal information is included.
Funding
This work did not receive funding.
Authors’ Contributions
S. Petrillo and L. Saccone: study design, manuscript draft.
C. Caria: study design, manuscript revision.
F. Franceschi and S. Romagnoli: manuscript revision, supervision.
All authors provided final approval of the version of the article to be published.
ORCID ID
S. Petrillo: 0000-0003-0843-2273
L. Saccone: 0000-0001-8660-3213
C. Caria: 0009-0008-0819-343X
F. Franceschi: 0000-0003-3917-8511
S. Romagnoli: 0000-0003-0152-4255
Conflict of Interest
All authors have no conflict of interest to disclose.
Data Availability
Data sharing does not apply to this article as no datasets were generated or analyzed during the current study.
AI Disclosure
Artificial intelligence was not used to create any original intellectual content presented in this article.
References
- Morgan-Jones R, Oussedik SI, Graichen H, Haddad FS. Zonal fixation in revision total knee arthroplasty. Bone Joint J 2015; 97: 147-149.
- Haidukewych GJ, Hanssen A, Jones RD. Metaphyseal fixation in revision total knee arthroplasty: indications and techniques. J Am Acad Orthop Surg 2011; 19: 311-318.
- Carender CN, An Q, Tetreault MW, De A, Brown TS, Bedard NA. Use of Cementless Metaphyseal Fixation in Revision Total Knee Arthroplasty in the United States. J Arthroplasty 2021; 37: 554-558.
- Nadorf J, Kinkel S, Gantz S, Jakubowitz E, Kretzer JP. Tibial revision knee arthroplasty with metaphyseal sleeves: The effect of stems on implant fixation and bone flexibility. PLoS One 2017; 12: e0177285.
- Stefani G, Mattiuzzo V, Prestini G, Civitenga C, Calafiore R, Traverso F. Porous-Coated Metaphyseal Sleeves in Revision Total Knee Arthroplasty: Midterm Results. JOINTS 2019; 7: 135-140.
- Bugler KE, Maheshwari R, Ahmed I, Brenkel IJ, Walmsley PJ. Metaphyseal Sleeves for Revision Total Knee Arthroplasty: Good Short-Term Outcomes. J Arthroplasty. 2015; 30: 1990-1994.
- Gøttsche D, Lind T, Christiansen T, Schroder HM. Cementless metaphyseal sleeves without stem in revision total knee arthroplasty. Arch Orthop Trauma Surg 2016; 136: 1761-1766.
- Scior W, Chanda D, Graichen H. Are Stems Redundant in Times of Metaphyseal Sleeve Fixation? J Arthroplasty 2019; 34: 2444-2448.
- Graichen H, Scior W, Strauch M. Direct, Cementless, Metaphyseal Fixation in Knee Revision Arthroplasty With Sleeves-Short-Term Results. J Arthroplasty 2015; 30: 2256-2259.
- Fonseca F, Sousa A, Completo A. Femoral revision knee Arthroplasty with Metaphyseal sleeves: the use of a stem is not mandatory of a structural point of view. J Exp Orthop 2020; 7: 24.
- Awadalla M, Al-Dirini RMA, O’Rourke D, Solomon LB, Heldreth M, Rullkoetter P, Taylor M. Influence of stems and metaphyseal sleeve on primary stability of cementless revision tibial trays used to reconstruct AORI IIB defects. J Orthop Res 2019; 37: 1033-1041.
- Frehill B, Crocombe AD. Finite element assessment of metaphyseal sleeves in total knee arthroplasty. J Orthop 2020; 19: 1-8.
- Bensmann G. Cementless fixation of endoprostheses. Biomed Tech (Berl) 2020; 3: 44-47.
- Parfitt AM. Targeted and nontargeted bone remodeling: relationship to basic multicellular unit origination and progression. Bone 2020; 30: 5-7.
- Holt G, Murnaghan C, Reilly J, Meek RM. The biology of aseptic osteolysis. Clin Orthop Relat Res 2007; 460: 240-252.
- Roodman GD. Advances in bone biology: the osteoclast. Endocr Rev 1996; 17: 308-332.
- Engh CA, O’Connor D, Jasty M, McGovern TF, Bobyn JD, Harris WH. Quantification of implant micromotion, strain shielding, and bone resorption with porous-coated anatomic medullary locking femoral prostheses. Clin Orthop Relat Res 1992; 285: 13-29.
- Jasty M, Bragdon C, Burke D, O’Connor D, Lowenstein J, Harris WH. In vivo skeletal responses to porous-surfaced implants subjected to small induced motions. J Bone Joint Surg Am 1997; 79: 707-714.
- Pilliar RM, Lee JM, Maniatopoulos C. Observations on the effect of movement on bone ingrowth into porous-surfaced implants. Clin Orthop Relat Res 1986; 208: 108-113.
- Sadoghi P, Liebensteiner M, Agreiter M, Leithner A, Bohler N, Labek G. Revision surgery after total joint arthroplasty: a complication-based analysis using worldwide registers. J Arthroplasty 2013; 28: 1329-1332.
- Barrack RL, Stanley T, Burt M, Hopkins S. The effect of stem design on end-of-stem pain in revision total knee arthroplasty. J Arthroplasty 2004; 19: 119-124.
- Gobba MS, Chan N, Patel R, Noble PC, Incavo SJ. Tibial Stems in Revision Total Knee Arthroplasty: Is There an Anatomic Conflict? J Arthroplasty 2015; 30: 86-89.
- Bieger R, Huch K, Kocak S, Jung S, Reichel H, Kappe T. The influence of joint line restoration on the results of revision total knee arthroplasty: comparison between distance and ratio-methods. Arch Orthop Trauma Surg 2014; 134: 537-541.
- Shen C, Lichstein PM, Austin MS, Sharkey PF, Parvizi J. Revision knee arthroplasty for bone loss: choosing the right degree of constraint. J Arthroplasty 2014; 29: 127-131.
To cite this article
Use of stem with metaphyseal sleeves in revision total knee arthroplasty: is it worth the hassle? a systematic review
JOINTS 2025;
3: e1649
DOI: 10.26355/joints_20259_1649
Publication History
Submission date: 31 Jul 2024
Revised on: 17 Sep 2024
Accepted on: 05 Sep 2025
Published online: 18 Sep 2025