JOINTS 2023;
1: e768
DOI: 10.26355/joints_202311_768
Adductor Longus proximal tears: a report of non-surgical treatment in 3 professional athletes
Topic: Sport Medicine
Category: Case report
Abstract
BACKGROUND: Although proximal adductor longus injuries have been recognized as the most common injuries of the medial compartment of the thigh, proximal injuries represent a small proportion. They frequently occur in athletes and can lead to significant loss of time from training or competition. Both conservative and operative treatments have been described in the literature. However, the management of these injuries remains controversial. Surgical treatment was previously preferred due to the common thought that only by restoring the anatomical length, the muscle would function properly, especially when significant retraction was present. The current study aimed to present a conservative treatment approach for proximal adductor longus injuries in elite athletes with a complete functional recovery.CASE SERIES: In this article, we present three cases of professional athletes who experienced a Munich Type 4 adductor longus proximal injury. After physical examination, MRI examinations showed a retraction of 4.85 cm (first case), 2.3 cm (second case), and 1 cm (third patient). Patients underwent conservative treatment and followed a strict return to play protocol that allowed them to return to competition between 2 and 4 months after injury, respectively, without any deficit.
CONCLUSIONS: Severe proximal adductor longus injuries in athletes can be treated nonoperatively while still achieving complete recovery in terms of strength and performance and avoiding the complications associated with surgery.
Background
Muscle injuries are a common occurrence in the athletic population, often resulting in significant disruptions to their training and competitive activities. These injuries typically result from overstretching or tearing of the muscle during incongruous movements, and they are often due to factors such as fatigue, overuse, or strength imbalances between propulsive and stabilizing muscles1.
A hip muscle injury that warrants attention is the adductor longus injury, which, although less common among muscle injuries, stands as the most prevalent injury within the medial compartment of the thigh, making it a leading cause of acute groin pain2. Although there have been reports in literature of injuries to both the proximal and distal adductor longus muscle, most injuries occur proximally to the musculotendinous junction. Notably, this injury is frequently reported3,4 in male athletes, particularly those engaged in ice hockey and soccer. Preliminary symptoms such as abdominal or groin pain are common in patients with this injury5,6. Most commonly, athletes present with pain localized to the adductor longus insertion on the pubic bone, both during palpation and with resistance testing7. Palpation of the adductor longus and other overall groin structures can be uncomfortable and often painful, even in the absence of injury. Therefore, the clinical tests should always be compared with the uninjured side. It is also important to consider that adductor-related groin pain often co-exists with other entities of groin pain8. Physical exam findings may also include a limited range of motion and swelling of the inner thigh9,10. The clinical examination should be supported by appropriate radiologic studies that allow early detection and precise morphologic description of the lesion. MRI is considered the gold standard imaging modality, providing detailed information on both bony and insertional structures11-13. One of its major advantages is its high sensitivity for both musculoskeletal and visceral lesions, pubic symphysis effusion, and bone marrow edema14.
The Munich Consensus Statement is one of the most popular methods for classifying acute muscle disorders and injuries. The classification of a structural myotendinous injury according to the Munich Consensus is described as follows15:
– Type 3A: Minor partial muscle tear;
– Type 3B: Moderate partial muscle tear;
– Type 4: Sub/total muscle tear or tendon avulsion.
The management of proximal tears of the adductor longus remains a subject of debate. In elite athletes, the treatment of acute hip adductor longus ruptures includes both surgical and non-surgical approaches10.
Surgical intervention has previously been advocated10 due to its potential benefits in restoring the natural working length of the muscle and facilitating the evacuation of extensive hematomas, thereby minimizing complications like myositis ossificans. However, nonoperative management offers the advantage of avoiding surgical risks while still enabling complete healing and recovery of strength. It is worth noting that some authors attribute continued groin pain and decreased functionality to conservative treatment10.
The non-operative treatment of adductor longus tears can be generally categorized into different phases. These phases are designed to minimize pain, restore a normal range of motion, enhance muscular strength, and facilitate a full return to previous levels of activity.
Phase 1: Acute phase (days 1-4/7)
The initial phase focuses on pain control and minimization of inflammation.
Phase 2: Sub-acute phase (weeks 1-4)
Recover flexibility and achieving isometric inner range (0-20°) adductor tendon strength concentric are the goals in this phase. Gentle isometric exercises and range of motion exercises are initiated. Passive stretching is also incorporated but with caution to prevent any exacerbation of the tear.
Phase 3: Remodeling phase (weeks 3-5)
The goal of this phase is to achieve a lower extremity passive range of motion equal to the unaffected side and an adductor strength in the inner range of at least 75% of the contralateral side. This phase involves the initiation of concentric and eccentric muscle training to strengthen the adductor muscles. Manual resistance exercises can also be introduced at this stage, as can sport-specific exercises, depending on the progress.
Phase 4: Functional phase (weeks 6-8)
The goal is to achieve an adduction strength of at least 90% to 100% with respect to the contralateral side in the inner range and 80% in the mid-range. Also, the goal is to reach a comparable strength of unaffected muscles on both limbs. The focus shifts to neuromuscular control and advanced strengthening exercises. More dynamic and plyometric exercises are included to prepare the individual for a return to full activity.
Once strength and range of motion are fully restored, and pain is minimal to non-existent, a graded return to sports or rigorous activity is undertaken. The return is closely monitored to ensure there is no recurrence of symptoms.
The current study aims to present a conservative treatment approach for proximal adductor longus injuries in elite athletes. Patients were evaluated through multiple parameters – clinically via physical examinations and strength tests, radiologically using MRI, and functionally through the Copenhagen Hip and Groin Outcome Score (HAGOS). This comprehensive evaluation proposes to provide insight into injury severity and rehabilitation effectiveness. All participants have provided informed consent for their data to be used for research purposes in compliance with ethical standards.
Case 1
The first case involved an 18-year-old professional youth national team soccer player who had been injured during training at the beginning of a running sprint. He described an audible “pop” and immediate pain along the proximal medial right thigh, which forced him off the playing field.
The clinical examination demonstrated significant swelling in the proximal groin near the pubic bone, which progressed to a large hematoma that spread down the medial and posterior thigh over the next few days. Severe pain was present on palpation of the proximal groin at the origin of the adductor longus. Attempted resisted contraction of the adductor longus was limited by severe pain at the proximal origin site. Sharp pain persisted for the first 48 hours, then slowly diminished. The player underwent RICE protocol (rest, ice, compression, elevation). Protected weight bearing and ambulation were allowed using two crutches. Seven days after the injury, he had an MRI showing a Type 4 lesion, according to Munich consensus15 (Sub/total muscle tear or tendon avulsion) of the adductor longus in its proximal part with a defect of 4.85 cm (Figure 1).
Figure 1. Coronal (a) and axial (b) PD FS MR images show a complete tear of the right adductor longus tendon, resulting in a 4.85 cm gap filled with fluid collection.
Note associated mild intramuscular and surrounding soft tissue edema.

After the MRI evaluation, he initiated the rehabilitation program described in Table 1. Due to the severity of the injury, however, the timeline of the 4 phases described in Table 1 was redefined according to the following scheme: phase 1 (0-15 days), phase 2 (15-40 days), phase 3 (40-90 days), and phase 4 (90-120 days).
Table 1. Rehabilitation program outline.
| Phase 1 – Acute phase
(0-10 days) |
RICE (Rest, Ice, Compression, Elevation)
Nonsteroidal Anti‐inflammatory Drugs Lymphatic drainage Stationary cycling Cryotherapy |
| Phase 2 – Subacute phase
(10-20 days) Goal: Concentric adduction against gravity without pain
|
Electrotherapy
Passive static stretching (gentle adductor stretch) Soft tissue mobilization Gym exercises (elliptical, cycling + light adductor isometric strengthening in the antigravity position (all except abduction) pain-free, low load, high repetition) |
| Phase 3 – Remodelling phase
(20-35 days) Goal: To restore a lower extremity passive range of motion equal to the uninvolved side; adductor strength at least 75% in respect to contralateral |
Electrotherapy
Running Dynamic stretching (gentle adductor stretch) Sport-specific balance/proprioceptive exercises Sumo squats Gym exercises (light adductor isotonic strengthening: concentric adduction with weight against gravity) |
| Phase 4 – Functional phase
Return to play (35-60 days) Goal: Adduction strength at least 90‐100% of the abduction strength and involved muscle strength equal to that of the contralateral side |
Sport-specific functional running exercises/drills (on the pitch)
3 times/week gym (strengthening phase II exercises with an increase in load, intensity, speed and volume) Dynamic stretching |
At 12 weeks after injury, the patient underwent a second MRI (Figure 2), which demonstrated absorption of the hematoma and satisfactory healing of the lesion on MRI without evidence of ossifying lesions. Manual testing of the adductor muscle performed at 12 weeks elicited no pain and showed strength equal to the contralateral side. The patient was then able to start phase 4 of the rehabilitation protocol with soccer-specific training. At 4 months after the injury, the patient was able to participate in an official match of the National Under-19 team.
Figure 2. Coronal PD FS (a) and axial PD (b) MR images of the same patient as Figure 1 were obtained 12 weeks after injury. Images demonstrate restored right adductor longus tendon continuity, with the previous gap filled with hypointense and slightly inhomogeneous scar tissue/neotendon.

Case 2
The second case involved a 33-year-old Olympic fencer who sustained an injury 2 months before the Olympic games. The injury mechanism was typical of the “lunge” – a noncontact, eccentric load with forced abduction and extension of the hip. This event resulted in acute disabling pain in the groin and proximal thigh, and he was unable to continue training. The patient had no history of groin pain or adductor issues before this injury.
On clinical examination, swelling, tenderness, and an extensive hematoma were noted in the left groin and the thigh. Palpation of the proximal origin of the adductor longus, as well as passive abduction and resisted adduction, resulted in pain. Adductor weakness was present on manual strength testing. The player underwent RICE protocol (rest, ice, compression, elevation). Protected weight bearing and ambulation were allowed using two crutches. An MRI performed 7 days after injury revealed a Type 4 lesion of the proximal adductor longus with a gap of 2.3 cm.
He underwent the protocol described in Table 1 and tolerated it well. He performed a second MRI one month after the injury, which showed an approximately 50% reduction in the lesion gap (1 vs. 2.3 cm) with the simultaneous appearance of inhomogeneous hypointense tissue, findings consistent with partial healing. Two months after injury, clinical evaluation demonstrated full recovery of muscle function without pain, and he was able to return to full participation. He recovered in time to participate in the Olympics and was able to medal in fencing.
Case 3
The third presented case involves a 33-year-old professional weightlifter who sustained a significant groin injury during a training session. While executing a single leg press, he experienced sudden and severe pain in the proximal adductor region accompanied by an audible popping sensation. He promptly stopped the session due to the pain and inability to bear weight on the affected leg. Notably, this patient had a history of persistent adductor tendon discomfort, which had never before necessitated a complete halt in training. Four days following the injury event, the patient underwent an MRI, which revealed a 10-mm Type 4 lesion of the left adductor longus tendon (Figure 3).
Figure 3. Sagittal T2w (a), coronal STIR (b), and axial T2w (c) MR images show a complete tear of the left adductor longus tendon, resulting in a 10 mm fluid gap with coexisting mild intramuscular and intermuscular edema.

The first assessment included muscle strength and passive flexibility testing, both inducing pain across various hip and knee positions. The baseline HAGOS was 10%, and palpation of the groin area evoked discomfort with no appearance of hematoma.
The rehabilitation protocol, depicted in Table 2, initiated seven days post-injury, implied two distinct isometric exercises for the adductor muscles in inner positions. Each day, once a day, these included five sets of 20-second isometric contractions. This approach was intentionally designed to maintain contractions under 20 seconds in adherence to the stress shielding principle, aiming to promote load-bearing without inducing excessive stress on the healing zone. These exercises were performed in the supine position with the knee flexed and extended, using a sphygmomanometer (Gima Italy, Milan, Italy). The sphygmomanometer served as both a resistance and measurement tool for adductor strength. Isometric contractions were performed against the resistance provided by the sphygmomanometer, which simultaneously measured the force exerted in millimeters of mercury (mmHg) (Figure 4).
Table 2. Rehabilitation program outline.
| Phase 1 – Acute phase
(0-4 days) |
RICE (Rest, Ice, Compression, Elevation)
Cryotherapy |
| Phase 2 – Subacute phase
(4-30 days) Goal: Recover flexibility and isometric inner range (0-20°) adductor tendon strength
|
Electrotherapy
Soft tissue mobilization Gym exercises (bike, hip thrust, dead bug, plank, knee extensor/flexor) Isometric adductor with sphygmomanometer, maximum tolerated intensity with knee in flexed and extended position |
| Phase 3 – Remodelling phase
(30-60 days) Goal: Lower extremity passive range of motion equal to the uninvolved side and involved adductor strength at least 75% in the inner range |
Electrotherapy
Running Dynamic stretching (gentle adductor stretch) Romanian Deadlifts, kneeling squat, Isotonic abdominal exercise Isotonic adductor exercise 0-45° Light adductor isotonic strengthening: side lying hip adduction against gravity and adding weight on ankle and standing adductor cable machine |
| Phase 4 – Functional phase
(60-90 days) Return to play Goal: Adduction strength at least 90% in inner position and 80% in mid-range position |
Sport-specific functional running exercises/drills (on the pitch)
2 times/week Gym Adductor isotonic strength (Copenhagen plank progression and Slider Squat with elastic resistance) (Figure 6) Resistance exercise: Barbell squat and deadlift |
| Phase 5 – Functional Phase
(90-120 days) Return to play Goal: Full Strength recovery |
Plyometric exercise
Adductor specific plyometric exercise Adductor full range strength Normal lower body training |
Figure 4. Isometric contraction with sphygmomanometer in knee extension (a) or flexion (b).

Gradually increasing the intensity, registered in mmHg, to an acceptable pain level was a key aspect of the rehabilitation process. Additionally, the patient engaged in isometric training for other muscle groups, including the upper body, abdominal muscles (e.g., plank or deadbug), gluteal muscles (hip thrust), knee flexors/extensors, and calf muscles, all following a “pain monitoring model”.
Positive progress was observed, with the patient experiencing pain-free walking after 10 days. Subsequent follow-ups showed improvement in the HAGOS score, hip abduction range of motion, and adductor muscle strength (Figure 5). The progression at clinical examination is displayed in Table 3.
Figure 5. a, Lying adductor stretch test using a smartphone. b, Lying hip adductor isometric test using a handheld dynamometer.

Table 3. LSI, limb-symmetry index.
| 1st month | 2nd month | 3rd month | 4th month | |
| HAGOS score, % | 61.1 | 72.8 | 83.2 | 95 |
| Isometric adductor strength, N | -95 | -50 | -14 | |
| LSI, % | 52.5 | 75 | 93 | 100 |
| Groin pain | Groin discomfort caused by end-range isometric contraction of the abdominal muscle | None | None | None |
| Hip abduction ROM restriction, degrees | -46° | 0 | 0 | 0 |
N, Newtons. Isometric adductor strength and hip abduction are obtained by comparing the affected and unaffected sides.
Progressive exercise regimens, including isometric contractions and specific movements like Copenhagen Plank and slider squats, were introduced over subsequent weeks (Figure 6).
The last clinical and radiographic follow-up was performed 4 months after the injury. Clinically, the patient was pain-free, had a HAGOS score of 95%, and had a 100% limb symmetry index (LSI) in all strength tests except for the end-range strength, which showed a 78% LSI.
Figure 6. a-b, Adductor plyometrics: side jump; (c), Copenhagen plank progression with hip overload.

MRI showed resolution of the edema and partial reattachment of the left adductor longus tendon to the pubic bone (Figure 7).
Finally, the patient resumed sport-specific movements and gradually recovered the load he was accustomed to before the injury.
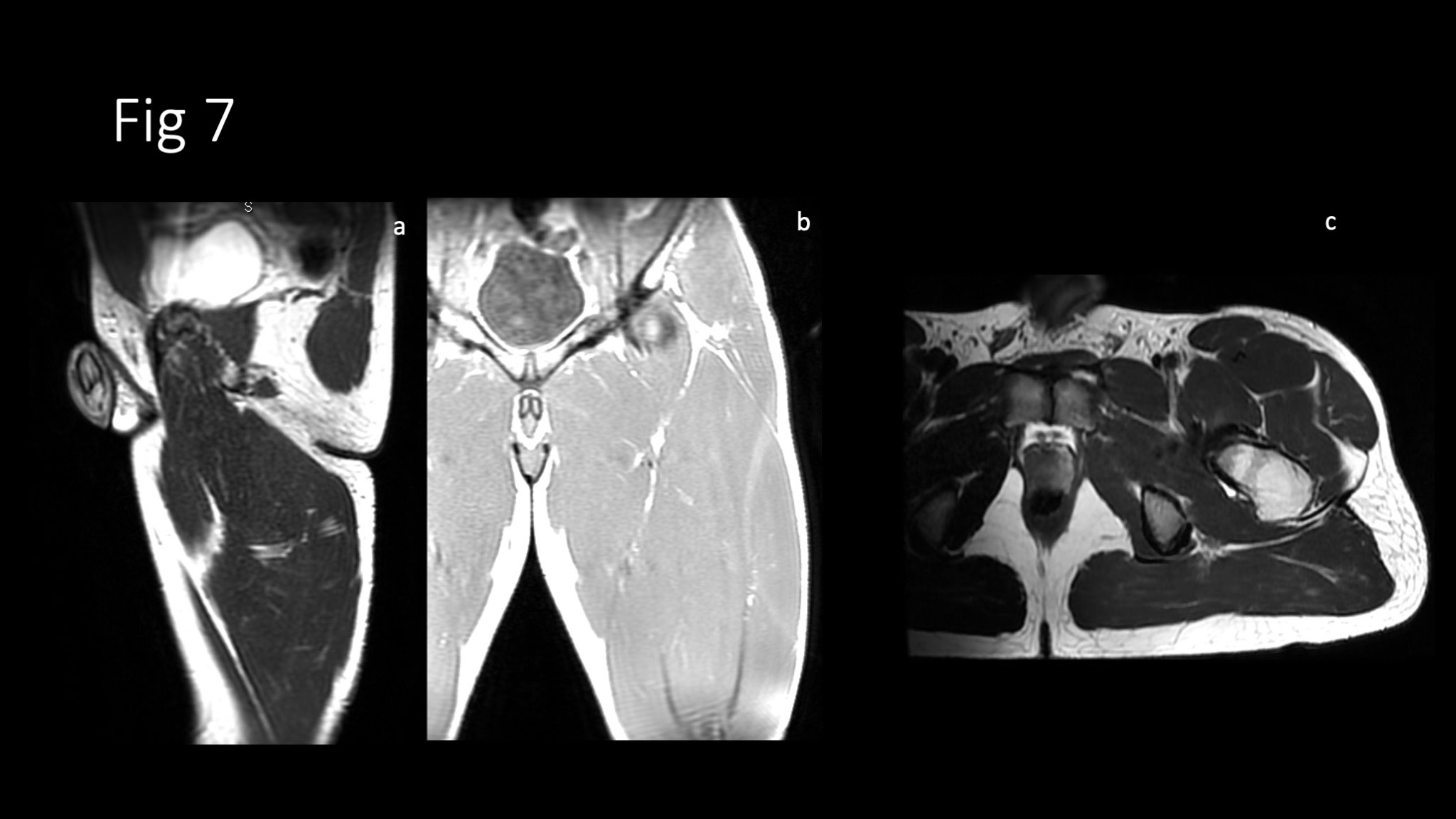
Figure 7. Sagittal T2w (a), coronal T1w (b), and axial T2w (c) MR images of the same patient as Figure 3. Follow-up MR exam obtained 16 weeks after injury shows partial reattachment of the left adductor longus tendon to the pubic bone with a residual tendon fibers discontinuity on the axial plane. Note the resolution of intermuscular and intramuscular edema.
Discussion
This study provides a comprehensive discussion of the effective management of proximal adductor longus injuries in elite athletes through conservative measures and a strict return-to-play protocol. The patients demonstrated successful clinical and radiologic healing with a return to full activities after high-grade injuries.
The optimal management of proximal adductor longus injuries remains controversial.
Previously, surgery had been preferred to non-surgical treatment for large defects of proximal adductor longus injuries. A common argument was that only surgical fixation could lead to a full return to pre-injury play level. However, numerous studies10,14,16-19 have reported positive results regarding conservative treatment, even in the case of severe and retracted lesions. Ueblacker et al16 described several parameters on six patients with proximal adductor longus injuries: demographics, mechanism of injury, classification of injury severity, tendon retraction, size defect on MRI, and return to play. Although an average retraction of the avulsed tendon was reported to be 2.1±0.5 cm, follow-up MRIs demonstrated gradual reattachment of the tendon in all the cases considered. All athletes returned to full sports activity at the pre-injury level within 88.7±12.8 (range 75-110) days with no functional deficiencies and manual muscle strength equal to the contralateral side.
Schlegel et al10 evaluated 19 National Football League (NFL) athletes with proximal adductor longus tears, 14 of whom were managed nonoperatively and 5 surgically. The authors found that nonoperative treatment of proximal adductor tendon rupture avoids the risks associated with surgery while providing an equal likelihood of return to play at the professional level. Furthermore, conservative management results in a statistically significantly faster return to play compared to operative treatment in NFL players. Thorborg et al17 described a case of bilateral adductor longus proximal tear in a soccer player that was treated conservatively. The player was able to participate in a full soccer training session without experiencing pain 15 weeks after the first rupture, and 12 weeks after the second rupture. Full hip adductor muscle-strength recovery was obtained 52 weeks after the first rupture and 10 weeks after the second rupture. The study conducted by Serner et al18 in 2020 explored factors that influence the time required for athletes to RTS after sustaining acute adductor injuries treated with non-operative treatment. Three thresholds were set for RTS: clinical absence of pain, completion of controlled sports training, and first full team training. Findings from the study, which included 81 athletes, showed that proximal adductor longus were the most severe injuries, requiring up to 11 weeks for a full return to team training. Key predictors of a prolonged RTS were identified as pain upon palpation of the proximal adductor longus insertion, a palpable defect, and injury at the bone-tendon junction as seen on MRI. For athletes lacking these key clinical findings, the added value of MRI for predicting RTS time was minimal.
Recently, Migliorini et al19 systematically reviewed the management of proximal adductor longus avulsion injuries in athletes. The final population included 46 male athletes averaging 30 years of age with a mean follow-up of 24.6 months. The mean stump retraction in surgically managed cases was found to be greater (3.3±0.6 cm) compared to conservatively managed cases (1.7±0.6 cm), although this did not reach statistical significance (p=0.07). Both surgical and conservative management yielded similar rates of return to pre-injury activity levels. However, the surgically managed cohort took significantly longer to return to sport (3.9±1.5 months vs. 2.2±1.0 months, p=0.0001). Thus, the study suggests that conservative management may offer a more expedient return to sports, albeit without compromising the achievement of pre-injury activity levels.
Lempainen et al20 investigated the surgical repair of complete proximal avulsion injuries of the adductor longus in a large population of athletes. The study reported that 90% of the 40 athletes observed experienced good to excellent functional outcomes following surgical repair, particularly when surgery was conducted sooner post-injury. However, no significant differences were found in relation to age at injury or preinjury Tegner score. The findings suggested that early surgical intervention might be beneficial for high-level athletes suffering from complete proximal adductor longus tears.
Different studies20-22 have used the injury gap as a criterion for surgical indication in complete adductor longus tears. Bharam et al21 recommended surgery when the retraction on MRI was <1 cm, whereas Best et al22 and Lempainen et al20 recommended surgery when the retraction was >2 cm. Contrasting results have been published12,23 regarding the injury gap as a negative prognostic factor. While Serner et al23 reported no effect of injury gap on the outcome of nonoperative treatment of complete ALM tears, Pezzotta et al12 found that a gap >2 cm was associated with delayed return to play. Patients included in the current study were referred for non-surgical treatment by presenting gaps between 1 and 4.85 cm.
The results of the 3 cases reported in the current study are comparable to the results of the recent literature describing non-surgical treatment of complete proximal adductor muscle injury, regardless of the amount of muscle retraction. Based on these findings, two factors commonly cited as reasons for surgical management of proximal adductor longus injuries (faster recovery and significant retractions) should be called into question. However, surgery could be considered a viable option if non-surgical treatment fails for 6 months or longer, or if the adductor longus injury occurs through the fibrocartilaginous enthesis3. A conservative approach should, therefore, be considered when treating high-level athletes with proximal adductor longus injuries. Non-surgical management may lead to an earlier full return to activity without functional deficits and avoids scar tissue or adhesions in the groin region and suture anchors in the pubic bone, which could cause further complaints in this sensitive area.
In this paper, we propose different approaches to the non-operative management of adductor longus tears. Individual differences in pain tolerance, injury severity, and healing rates will necessitate modifications in the rehabilitation process. Factors such as injury severity, patient age, and sport-specific demands could influence the choice between protocols. For example, the protocols outlined in Table 1 and Table 2 differ in their duration, exercises, and overall goals. While both protocols begin with an acute phase focused on RICE and progress to sport-specific exercises, the choice between them is influenced by determinants such as lesion severity, athlete age, and sport-specific requirements. For example, the protocol in Table 1 includes plyometric exercises in the final phase, making it more suitable for sports that require explosive movements. On the other hand, Table 2 uses isometric exercises, which may be more appropriate for sports that require sustained muscle contractions.
Conclusions
Severe injuries to the proximal adductor longus can be managed non-surgically, even in professional athletes, with a complete recovery in muscular strength and athletic performance. Surgical interventions and their associated complications could thus be avoided. It is imperative, however, to transparently communicate to the athlete during the initial diagnostic phase that the median duration for full recovery is estimated to be around 12 weeks.
Conflict of Interest
The authors declare no conflicts of interest.
Informed Consent
All participants have provided informed consent for their data to be used for research purposes in compliance with ethical standards.
Ethics Approval
Not applicable.
Funding
None.
Data Availability
Data are available upon request.
ORCID ID
Alessandro Carrozzo: 0000-0003-0700-8139.
References
- Garrett WE, Safran MR, Seaber AV, Glisson RR, Ribbeck BM. Biomechanical comparison of stimulated and nonstimulated skeletal muscle pulled to failure. Am J Sports Med 1987; 15: 448-454.
- Macintyre J, Johson C, Schroeder EL. Groin Pain in Athletes. Curr Sports Med Rep 2006; 5: 293-299.
- Nicholas SJ, Tyler TF. Adductor Muscle Strains in Sport. Sports Med 2002; 32: 339-344.
- Dimitrakopoulou A, Schilders EMJ, Talbot JC, Bismil Q. Acute Avulsion of the Fibrocartilage Origin of the Adductor Longus in Professional Soccer Players: A Report of Two Cases. Clin J Sport Med 2008; 18: 167-169.
- Tansey RJ, Benjamin-Laing H, Jassim S, Liekens K, Shankar A, Haddad FS. Successful return to high-level sports following early surgical repair of combined adductor complex and rectus abdominis avulsion. Bone Joint J 2015; 97: 1488-1492.
- Bisciotti GN, Chamari K, Zini R, Corsini A, Auci A, Bisciotti AL, Bisciotti AN, Cena E, Rodriguez Garcia G, Volpi P, Vuckovic Z, Canata GL. Adductor longus tenotomy in the treatment of groin pain syndrome in athletes: a systematic review. JOINTS 2023; 1: e602.
- Hölmich P. Long-standing groin pain in sportspeople falls into three primary patterns, a “clinical entity” approach: a prospective study of 207 patients. Br J Sports Med 2007; 41: 247-252.
- Zwerver J, Brink M, Cook J. Tendon injuries in football players: FC barcelona 2021 tendon guide. https://www.lasselempainen.fi/tendon-injuries-in-football-players-fc-barcelona-2021-tendon-guide/?lang=en. Accessed on 21 October 2023.
- Verrall GM, Hamilton IA, Slavotinek JP, Oakeshott RD, Spriggins AJ, Barnes PG, Fon GT. Hip joint range of motion reduction in sports-related chronic groin injury diagnosed as pubic bone stress injury. J Sci Med Sport 2005; 8: 77-84.
- Schlegel TF, Bushnell BD, Godfrey J, Boublik M. Success of Nonoperative Management of Adductor Longus Tendon Ruptures in National Football League Athletes. Am J Sports Med 2009; 37: 1394-1399.
- Zoga AC, Mullens FE, Meyers WC. The spectrum of MR imaging in athletic pubalgia. Radiol Clin North Am 2010; 48: 1179-1197.
- Pezzotta G, Pecorelli A, Querques G, Biancardi S, Morzenti C, Sironi S. MRI characteristics of adductor longus lesions in professional football players and prognostic factors for return to play. Eur J Radiol 2018; 108: 52-58.
- Drogo P, Carrozzo A, Partezani Helito C, Zappalà G, Barelli GM, Argento G, Ferretti A, Monaco E. Magnetic resonance imaging evaluation of anterolateral ligament injuries and associated lesions in acute anterior cruciate ligament tears. JOINTS 2023; 1: e676.
- Koulouris G. Imaging review of groin pain in elite athletes: an anatomic approach to imaging findings. AJR Am J Roentgenol 2008; 191: 962-972.
- Mueller-Wohlfahrt HW, Haensel L, Mithoefer K, Ekstrand J, English B, McNally S, Orchard J, van Dijk CN, Kerkhoffs GM, Schamasch P, Blottner D, Swaerd L, Goedhart E, Ueblacker P. Terminology and classification of muscle injuries in sport: The Munich consensus statement. Br J Sports Med 2013; 47: 342-350.
- Ueblacker P, English B, Mueller-Wohlfahrt HW. Nonoperative treatment and return to play after complete proximal adductor avulsion in high-performance athletes. Knee Surg Sports Traumatol Arthrosc 2016; 24: 3927-3933.
- Thorborg K, Petersen J, Nielsen MB, Hölmich P. Clinical recovery of two hip adductor longus ruptures: a case-report of a soccer player. BMC Res Notes 2013; 6: 205.
- Serner A, Weir A, Tol JL, Schilders E, Mosler A, Whiteley R, Thorborg K, Robinson M, Hölmich P, Otten R. Associations Between Initial Clinical Examination and Imaging Findings and Return-to-Sport in Male Athletes With Acute Adductor Injuries: A Prospective Cohort Study. Am J Sports Med 2020; 48: 1151-1159.
- Migliorini F, Maffulli N, Eschweiler J, Tingart M, Baroncini A. Surgical versus conservative management of traumatic proximal adductor longus avulsion injuries: A systematic review. Surgeon 2022; 20: 123-128.
- Lempainen L, Hetsroni I, Kosola JA, Sinikumpu JJ, Mazzoni S, Orava S. Proximal Adductor Longus Tendon Repair With a Concomitant Distal Fascial Release for Complete Hip Adductor Tendon Tears: Surgical Technique and Outcomes in 40 Male Athletes. Orthop J Sports Med 2021; 9: 23259671211042024.
- Bharam S, Feghhi DP, Porter DA, Bhagat PV. Proximal Adductor Avulsion Injuries: Outcomes of Surgical Reattachment in Athletes. Orthop J Sports Med 2018; 6: 232596711878489.
- Best R, Gild A, Huth J, Beckmann J. Patient-related outcome measurements after operative and conservative management of traumatic proximal adductor longus avulsion injuries. Int Orthop 2020; 44: 965-971.
- Serner A, Hölmich P, Arnaiz J, Tol JL, Thorborg K, Weir A. One-Year Clinical and Imaging Follow-up After Exercise-Based Treatment for Acute Complete Adductor Longus Tendon Avulsions in Athletes: A Prospective Case Series. Am J Sports Med 2021; 49: 3004-3013.
To cite this article
Adductor Longus proximal tears: a report of non-surgical treatment in 3 professional athletes
JOINTS 2023;
1: e768
DOI: 10.26355/joints_202311_768
Publication History
Submission date: 15 Sep 2023
Revised on: 25 Sep 2023
Accepted on: 03 Nov 2023
Published online: 17 Nov 2023